Table of Contents >> Show >> Hide
- What are vital signs?
- Why vital signs matter (even when you “feel fine”)
- Normal adult vital sign ranges (quick reference)
- Blood pressure ranges: what the categories actually mean
- Pediatric vital signs: kids aren’t just “tiny adults”
- How to measure vital signs accurately at home
- What can change vital signs (without anything “being wrong”)
- When to be concerned (and when to get help)
- FAQs people actually ask
- Putting it all together: a simple way to think about vital signs
- Real-world experiences and stories (extra )
Think of vital signs as your body’s “dashboard lights.” They don’t tell you everything about what’s going on under the hood,
but they’re fantastic at answering one big question: “Are the basics running smoothly right now?”
In clinics, hospitals, schools, and even your living room (hello, home blood pressure cuffs), vital signs help spot early clues of infection,
dehydration, stress, asthma flare-ups, heart issues, and more. Sometimes they’re boring. Sometimes they’re the plot twist.
This article covers what vital signs are, typical adult and child ranges, what can throw them off, and how to make sense of the numbers
without spiraling into “I am definitely a medical mystery” territory.
What are vital signs?
Vital signs are basic measurements that reflect how well your body is doing its essential jobscirculating blood, breathing,
regulating temperature, and (in many settings) getting enough oxygen.
The “classic four” vital signs are:
- Body temperature (how warm you are)
- Pulse (heart rate) (how fast your heart beats)
- Respiratory rate (how fast you breathe)
- Blood pressure (how strongly blood pushes on artery walls)
Many healthcare teams also track:
- Oxygen saturation (SpO₂) (how much oxygen your blood is carrying)
- Pain score (often rated 0–10because “ow” is not a unit of measurement)
Why vital signs matter (even when you “feel fine”)
Vital signs can change before you notice symptoms. For example:
- Your temperature may rise early in an infectionsometimes before the sore throat announces itself.
- A fast heart rate can show up with dehydration, anxiety, fever, anemia, or after a triple-espresso decision you now regret.
- Blood pressure is famously sneakyoften high with no obvious symptoms, but still important to catch and manage.
- Oxygen saturation can drop with lung problems even when you’re trying to “walk it off.”
The key is context: one odd number isn’t automatically an emergency, but patterns and extremes deserve attention.
Normal adult vital sign ranges (quick reference)
“Normal” isn’t one magic number. It’s a range influenced by age, fitness, medications, stress, sleep, and whether someone just speed-walked
from the parking lot like it was an Olympic event. Still, here are commonly used resting adult ranges:
Adult vital signs at rest (typical ranges)
- Temperature: roughly 97°F to 99°F (about 36.1°C to 37.2°C)
- Heart rate (pulse): about 60 to 100 beats per minute
- Respiratory rate: about 12 to 20 breaths per minute (many references use 12–18)
- Blood pressure: generally above 90/60 and below 120/80
- Oxygen saturation (SpO₂): typically 95% to 100% for most healthy people
If you want an ultra-simple memory trick: most healthy adults at rest are around “98.6, 72, 16, 120/80, 98%”
(temperature, pulse, breathing, blood pressure, oxygen). Real life is messierbut that’s the vibe.
Blood pressure ranges: what the categories actually mean
Blood pressure is written as systolic/diastolic (for example, 118/76). Systolic is the pressure when the heart contracts;
diastolic is when the heart relaxes between beats.
Many U.S. health organizations use these adult categories:
- Normal: less than 120 systolic and less than 80 diastolic
- Elevated: 120–129 systolic and less than 80 diastolic
- Stage 1 hypertension: 130–139 systolic or 80–89 diastolic
- Stage 2 hypertension: 140+ systolic or 90+ diastolic
- Hypertensive crisis: 180+ systolic and/or 120+ diastolic (seek urgent care guidance)
Two important reality checks:
- One reading isn’t a diagnosis. Healthcare pros usually look for consistent patterns over time.
-
How you measure matters. Wrong cuff size, talking during the reading, legs crossed, or taking it right after stairs
can all inflate numbers.
Pediatric vital signs: kids aren’t just “tiny adults”
Kids’ bodies run fasterlike laptops with 37 tabs open and zero fear. So normal heart and breathing rates are often higher in infants and
gradually slow as children grow.
Below are general ballpark ranges used in many pediatric references. Your child’s clinician will interpret readings based on age,
health, and the situation.
Typical pediatric patterns (very general)
- Infants: higher heart rate and breathing rate are common
- School-age kids: rates trend closer to adult ranges
- Teens: often similar to adults (especially at rest)
Example ranges you may see referenced:
- Infant respiratory rate: often around 30–60 breaths/min
- Adolescent respiratory rate: often closer to 12–16 breaths/min
- Young child heart rate: commonly higher than adults; teens often overlap with adult 60–100 beats/min at rest
Translation: if you compare a toddler’s heart rate to an adult chart, you’ll scare yourself for no reason. Use age-appropriate references
and ask a clinician when you’re unsure.
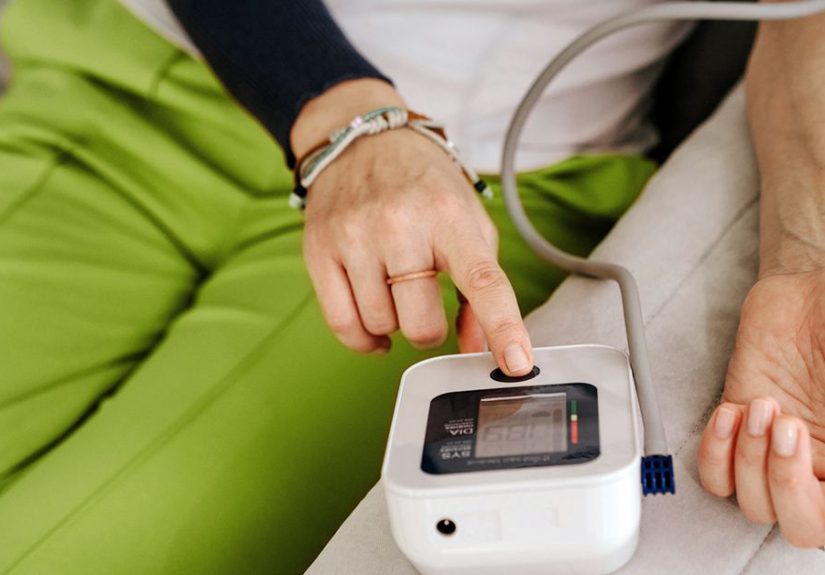
How to measure vital signs accurately at home
Home monitoring can be helpfulespecially for blood pressure, temperature, or oxygen saturationif you do it correctly. (If not, you’ll
mostly measure how powerful anxiety is.)
Temperature tips
- Follow the thermometer’s instructions (oral, ear, forehead, etc. can differ).
- Wait at least 15 minutes after hot/cold drinks before an oral temp.
- Take it at roughly the same time of day if you’re tracking trends.
Pulse (heart rate) tips
- Sit quietly for a few minutes first.
- Use your index and middle fingers (not your thumb) on the wrist or neck.
- Count beats for 30 seconds and multiply by 2 (or count for a full minute if it feels irregular).
Respiratory rate tips
- Measure at rest. Don’t do it right after rushing or laughing so hard you snorted.
- Count breaths for one full minute (one inhale + one exhale = one breath).
Blood pressure tips
- Sit with back supported, feet flat, arm supported at heart level.
- Rest quietly 5 minutes first; avoid caffeine/exercise/smoking right beforehand if possible.
- Use the right cuff size. Too small can read high; too large can read low.
- Take 2 readings about a minute apart and average them.
Pulse oximeter (SpO₂) tips
- Warm hands and remove nail polish if possible.
- Stay still and wait for the number to stabilize.
- Know that accuracy can varyespecially with poor circulation, movement, or certain device limitations.
A quick note on pulse oximeters: U.S. regulators have highlighted that some devices may show accuracy differences across skin tones and under
certain conditions. That doesn’t make them uselessit just means you should treat readings as one piece of the puzzle, not the entire mystery novel.
What can change vital signs (without anything “being wrong”)
Vital signs are sensitive. That’s their job. These common factors can shift numbers:
- Activity: exercise raises pulse and breathing; sometimes temperature too.
- Stress/anxiety: can raise heart rate and blood pressure (“white coat effect” is real).
- Sleep and fatigue: can affect pulse, blood pressure, and how you breathe.
- Hydration: dehydration can raise heart rate and lower blood pressure in some people.
- Medications: stimulants, decongestants, beta-blockers, and many others can shift readings.
- Age and fitness: athletes may have a lower resting heart rate; older adults may run cooler.
- Altitude: oxygen saturation can be lower at higher elevations.
This is why clinicians love trends. One “weird” reading can be noise; a consistent pattern is a message.
When to be concerned (and when to get help)
Vital sign numbers should be interpreted with symptoms and context. Still, some situations deserve prompt medical advice:
Call a healthcare professional urgently if you have:
- Very high blood pressure (especially around crisis-level numbers) with symptoms like chest pain, severe headache, confusion, or shortness of breath
- Oxygen saturation persistently low (especially with breathing trouble, bluish lips/face, or worsening symptoms)
- High fever that doesn’t improve or is paired with severe symptoms
- Very fast or very slow pulse with dizziness, fainting, chest pain, or severe weakness
For infants and very young children, fever and breathing concerns can be more urgentalways follow pediatric guidance and seek care sooner
rather than later if you’re worried.
FAQs people actually ask
Is 98.6°F the only “normal” temperature?
Nope. It’s a traditional average. Many healthy adults run a bit lower or higher depending on time of day, activity, and individual variation.
That’s why typical ranges matter more than one mythic number.
Why is my blood pressure higher at the doctor’s office?
You’re not alone. Anxiety, rushing, and even talking can nudge readings up. That’s one reason home monitoring (done correctly) can be helpful
for some peopleyour clinician can compare office and home patterns.
Why do kids have faster heart rates?
Growing bodies have different metabolic needs, and smaller hearts often beat faster to deliver oxygen and nutrients efficiently. As kids grow,
the “normal” range gradually shifts toward adult values.
Is pain really a “vital sign”?
In many healthcare settings, pain is routinely assessed alongside other vital signsoften using a 0–10 scale. The goal is to catch undertreated
pain and guide care. The best approach treats pain scores as meaningful information, but still considers the full clinical picture.
Putting it all together: a simple way to think about vital signs
Vital signs are less like a final exam and more like a group chat:
one number by itself can be misleading, but together they tell a story.
Example:
- If your temperature is up and your pulse is faster than usual, that could fit with a fever from an infection.
- If your oxygen saturation is normal but your respiratory rate is high after sprinting to catch the bus, that could just be… the bus.
- If your blood pressure is borderline high once, it may mean “recheck,” not “panic.” If it’s repeatedly high, it means “talk to your clinician.”
When you track vital signs at home, aim for calm, consistent techniqueand focus on trends. Your future self will thank you for the data that
isn’t sabotaged by caffeine, crossed legs, and an argument with your printer.
Real-world experiences and stories (extra )
To make vital signs feel less like a textbook and more like real life, here are a few common “this totally happens” scenarios people experience.
These aren’t personal medical advicejust relatable patterns clinicians hear about all the time.
1) The “white coat effect” moment
A lot of people swear their blood pressure is fineright up until a cuff squeezes their arm in a brightly lit room while someone asks,
“Any stress lately?” Suddenly, the numbers jump. That’s the white coat effect: being nervous (even mildly) can raise blood pressure and heart rate.
The funny part is that the anxiety sometimes comes from seeing the number that anxiety created.
A practical takeaway: if you’re monitoring at home, recreate the calmest conditions you cansit quietly for a few minutes, feet flat, arm supported,
no doom-scrolling. Taking two readings and averaging them can also reduce the “first reading drama.”
2) The “I’m not sick, I’m just dehydrated” plot twist
Someone spends a day running errands, forgets to drink water, and later feels lightheaded. Their heart rate is up. Maybe their blood pressure is a little lower than usual.
They take a temperature and it’s normal, so they’re confuseduntil they drink fluids and rest. Vital signs often react quickly to hydration levels, especially pulse.
The takeaway: if your pulse is higher than normal at rest, consider the basics firstwater intake, sleep, stress, and recent activitybefore you assume
something mysterious is happening.
3) The “fever math” experience
With a fever, people often notice a one-two combo: temperature rises and heart rate climbs. This can feel alarming if you’re not expecting it.
But it’s a common patternyour body is working harder. Many people also notice their breathing feels a bit faster. The key is watching the trend:
is the fever improving with rest and appropriate care, or is it persisting and paired with worsening symptoms?
The takeaway: write down readings with times (for example, “7:30 PM: 100.4°F, pulse 104”) so you can see whether you’re improving or not.
4) The pulse oximeter spiral (and how to avoid it)
Home pulse oximeters are popular because they’re easy. They’re also famous for causing unnecessary anxiety when the number flickers.
People often try it right after walking, with cold hands, or while movingthen see a random low reading and panic.
In reality, technique matters: warm hands, sit still, wait for the value to stabilize, and repeat once.
Another real-world detail: devices aren’t perfect, and accuracy can vary by device and conditions. If you feel fine and your readings bounce around,
focus on consistent technique and symptoms. If you feel short of breath or unwell, don’t let a “pretty number” talk you out of getting help.
5) The “kids are fast” reality check
Parents often notice their child’s heart beating quickly and assume something is wrongespecially after play, crying, or a fever.
In pediatrics, normal ranges are different and depend heavily on age. A toddler’s “normal” can look wild compared to an adult’s chart.
The most useful habit is tracking what’s normal for your child when they’re healthy, then noticing meaningful changes.
If there’s one big lesson from all these experiences, it’s this:
vital signs are most helpful when you treat them like informationnot a verdict.
Pair the numbers with context, technique, and common sense, and they become a powerful tool for understanding what your body is doing.