Table of Contents >> Show >> Hide
- The “20%” headline: what it really means (and what it doesn’t)
- Meet the SELECT trial: the study behind the heart-protection claim
- So… why would a weight-loss drug protect the heart?
- Which outcomes improved the most?
- Who might benefit mostand who should not use Wegovy
- Side effects and safety: the part nobody makes a cute TikTok about
- How to talk to your clinician about Wegovy like a pro (without being annoying)
- The big picture: why this matters
- Experiences: what taking Wegovy can feel like in real life (a 500-word, reality-based walkthrough)
- Conclusion
Imagine a weight-loss shot that doesn’t just help your jeans fit again, but also helps protect the organ
that has been loyally pumping through every “I’ll start Monday” phase of your life. That’s the headline
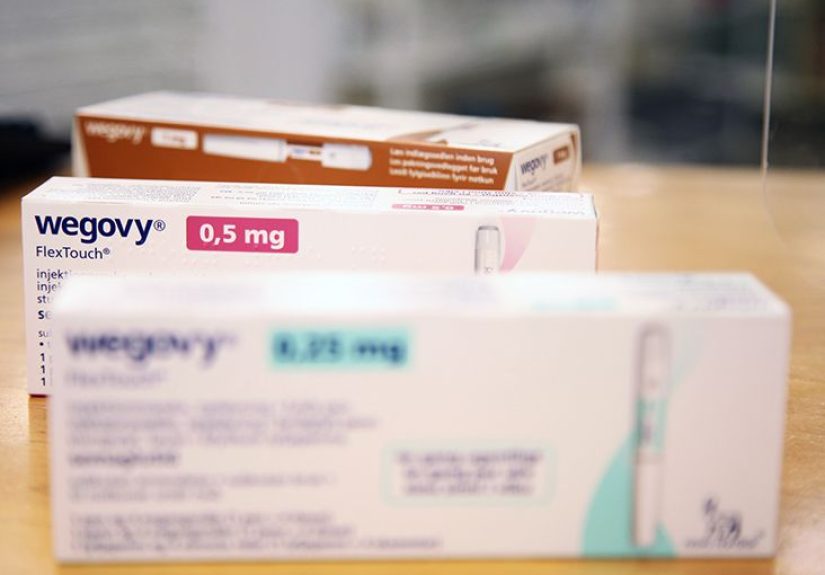
behind Wegovy (semaglutide): in a major clinical trial, people with overweight or obesity and established
cardiovascular disease had a 20% lower risk of major heart-related events while taking it.
Before we throw a ticker-tape parade made of salad greens, let’s unpack what that 20% actually means,
who it may help most, what the trade-offs look like, and how to talk to your clinician like a person who
read the whole article (instead of just texting the headline to the group chat).
The “20%” headline: what it really means (and what it doesn’t)
When you hear “Wegovy lowers heart attack and stroke risk by 20%,” that’s shorthand for a reduction in
major adverse cardiovascular events (often abbreviated as MACE). In the landmark SELECT trial,
MACE was defined as a composite of:
- Cardiovascular death
- Nonfatal heart attack (myocardial infarction)
- Nonfatal stroke
Over about 40 months of follow-up, 6.5% of people taking semaglutide had one of these events,
compared with 8.0% of people taking placebo. That’s the famous “20%” (a relative risk reduction; hazard ratio ~0.80).
But the absolute difference matters too: 1.5 percentage points over a little more than three years.
A practical way to think about it: if 100 people similar to those in SELECT took Wegovy, about 1–2 major
cardiovascular events might be prevented over roughly 3–4 years compared with placebo. Put differently,
the “number needed to treat” is in the neighborhood of ~67 people over that time frame to prevent one event
(based on the trial’s absolute difference).
That is still meaningfulespecially in a group already at high riskbut it’s not magic, and it’s not a force
field. Wegovy doesn’t replace statins, blood pressure control, smoking cessation, or cardiac rehab. It joins the
group chat and (when tolerated and used consistently) may make the whole plan work better.
Meet the SELECT trial: the study behind the heart-protection claim
SELECT wasn’t a small “we tried this on 38 people and everyone felt inspired” study. It was a large,
international, randomized, double-blind trial with 17,604 participants. Everyone had:
- Overweight or obesity (BMI ≥ 27)
- Established cardiovascular disease (prior heart attack, prior stroke, or symptomatic peripheral artery disease)
- No diabetes at enrollment (a key detail for how we interpret the evidence)
The average participant was about 62 years old, and roughly 28% were women. The mean BMI was
about 33, and most people were already on modern heart-protective therapyabout 88% were taking statins.
In other words, Wegovy’s benefit showed up on top of the usual “cardiology greatest hits.”
Dosing followed the familiar Wegovy ramp-up: a low weekly starting dose that was increased every four weeks
as tolerated, aiming for 2.4 mg once weekly. About 77% of participants reached the target dose.
One more nuance that matters: about two-thirds of participants had prediabetes (HbA1c 5.7–6.4) at baseline.
That becomes important when we talk about mechanisms, because preventing diabetes is itself a heart-protection strategy.
So… why would a weight-loss drug protect the heart?
Wegovy is a GLP-1 receptor agonist. In plain English: it mimics a gut hormone that helps regulate appetite,
slows gastric emptying, and influences brain pathways involved in hunger and satiety. Many people naturally eat
less because they feel full soonerand they feel less “food noise,” which is a surprisingly big deal if your brain
treats snack aisles like a haunted house you must enter to defeat your fears.
But the heart benefit probably isn’t just “the scale went down, therefore the risk went down.” In SELECT,
semaglutide was associated with:
- Meaningful weight loss: about 9.4% average body-weight reduction at 104 weeks (vs ~0.9% with placebo)
- Lower systolic blood pressure: about –3.8 mm Hg (vs –0.5 mm Hg)
- Far fewer people crossing into diabetes: HbA1c ≥ 6.5% occurred in 3.5% on semaglutide vs 12.0% on placebo
Those shiftsweight, blood pressure, and metabolic healthare all proven cardiovascular levers. There’s also
growing scientific discussion about additional effects of GLP-1 therapies on inflammation, endothelial function,
and atherosclerosis biology. We don’t need to claim a single “secret mechanism” to appreciate the likely reality:
it’s probably multifactorial.
Which outcomes improved the most?
The primary composite outcome improved. But when you zoom in, some pieces moved more than others:
-
Nonfatal heart attack was lower with semaglutide (about 2.7% vs 3.7%).
That’s one of the clearer “component wins.” - All-cause death was also lower (about 4.3% vs 5.2%), suggesting benefits that go beyond a single endpoint definition.
- Cardiovascular death trended lower (about 2.5% vs 3.0%), though this particular component did not hit conventional statistical significance on its own.
- A composite related to heart failure outcomes (CV death or heart-failure hospitalization) was also improved (about 3.4% vs 4.1%).
Translation: the 20% headline isn’t one lucky coin flip; multiple clinically important outcomes generally
leaned in the right direction.
Who might benefit mostand who should not use Wegovy
The FDA-approved “heart risk reduction” use
In March 2024, the FDA approved Wegovy to reduce the risk of major cardiovascular events (cardiovascular death,
nonfatal heart attack, and nonfatal stroke) in adults with established cardiovascular disease and either
obesity or overweight, alongside a reduced-calorie diet and increased physical activity.
That’s a specific population: this is not “everyone who wants to be beach-ready by Memorial Day.”
It’s a secondary-prevention toolmeaning it’s meant for people who already have cardiovascular disease,
where preventing the next event is the goal.
People who should avoid Wegovy (or need very careful evaluation)
Wegovy carries a boxed warning about the risk of thyroid C-cell tumors based on animal studies and is
contraindicated in people with a personal or family history of medullary thyroid carcinoma or
Multiple Endocrine Neoplasia syndrome type 2 (MEN 2).
It also isn’t recommended to combine Wegovy with other semaglutide-containing products or other GLP-1 receptor agonists.
And as with any prescription therapy, pregnancy planning, pancreatitis history, gallbladder disease history,
severe gastrointestinal disease, and kidney risks all deserve a clinician-led conversation.
Side effects and safety: the part nobody makes a cute TikTok about
If Wegovy had a personality, it would be “very effective, occasionally dramatic.” The most common issues are
gastrointestinalnausea, vomiting, diarrhea, constipation, abdominal discomfort, and heartburn-type symptoms.
In SELECT, discontinuation due to adverse events was higher with semaglutide:
16.6% stopped the study drug versus 8.2% on placebo, and GI complications were more frequent.
The reassuring news from SELECT is that several serious adverse outcomes were not increased compared with placebo:
acute pancreatitis and acute kidney failure were similar between groups in the published summaries, and overall
serious adverse events were actually slightly lower with semaglutide.
Still, “not increased in a trial” doesn’t mean “impossible in real life.” The label and clinical guidance emphasize:
- Gallbladder problems (including gallstones), especially with rapid weight loss
- Dehydration-related kidney injury (often from persistent vomiting/diarrhea)
- Potential pancreatitis warning signs (severe, persistent abdominal painsometimes radiating to the back)
- Thyroid tumor warning signs (neck lump, hoarseness, trouble swallowing, shortness of breath)
None of this is meant to scare youit’s meant to make you a competent adult about it. Many people tolerate the medication
well once they get through the dose-escalation phase. Others decide the side effects aren’t worth it, or they need a slower
titration schedule. Both outcomes are valid. Your heart does not award bonus points for suffering.
How to talk to your clinician about Wegovy like a pro (without being annoying)
If you have established cardiovascular disease and you’re living with overweight or obesity, a smart conversation might include:
- “Do I meet the FDA-labeled criteria for cardiovascular risk reduction with Wegovy?”
- “What’s my baseline risk of another event in the next 3–5 years?” (This helps contextualize the absolute benefit.)
- “What side effects should I watch for, and what’s our plan if I can’t tolerate dose increases?”
- “How does this fit with my current meds?” (Especially if you’re on therapies that affect blood sugar.)
- “What lifestyle plan are we pairing with it?” (Because the medication is an assistant coach, not the whole team.)
Also helpful: ask about strategy, not just a prescription. Many people do better when they start with concrete tactics:
smaller meals, lower-fat foods during titration, consistent protein, more fiber and water, and a plan for constipation
(because nobody wants their fitness journey to become a plumbing emergency).
The big picture: why this matters
In the U.S., obesity remains common, and cardiovascular disease remains a leading cause of death. Even small shifts in risk
can translate into a large public health impact when applied to millions of high-risk adults. The significance of SELECT is that it
provided evidence that treating obesity pharmacologically can do more than change weightit can change hard cardiovascular outcomes
in a secondary-prevention population.
The “future headline” here isn’t just “people lost weight.” It’s: “we may have another tool to prevent the next heart attack or stroke
in people who already have cardiovascular disease.” That’s a different category of win.
Experiences: what taking Wegovy can feel like in real life (a 500-word, reality-based walkthrough)
Everyone’s experience with Wegovy is different, but patterns repeat often enough that clinicians can usually predict the “vibe.”
Here’s a composite, reality-based look at what many patients reportwithout pretending this is a universal script.
Week 1–4 (starting dose): The first surprise is how quickly appetite can change. Some people describe it as
“the volume got turned down” on constant food thoughts. You might notice you’re halfway through a meal and suddenly feel like
you’ve had enoughan unfamiliar sensation if you’re used to cleaning the plate out of habit. The less-fun part is nausea:
it can show up as mild queasiness, a “too full” feeling, or a sudden aversion to greasy foods. Many people learn fast that
a giant burger-and-fries combo on injection day is an ambitious choice. Smaller portions, slower eating, and avoiding high-fat meals
can make the adjustment smoother.
Week 5–12 (dose escalation): This is where things can get dramatic. As the dose increases, side effects can
intensifyespecially if you jump your eating habits too quickly from “normal” to “I am still a human with a digestive system.”
Constipation is common, and it can be sneaky: you don’t always feel terrible, but you notice… delays. People who do best often
treat hydration like a daily assignment, add fiber gradually, and prioritize protein so weight loss doesn’t become muscle loss.
Social situations get interesting, too. Some people feel awkward ordering half a meal or skipping alcohol because it suddenly doesn’t
sound appealing. (Pro tip: “I’m working on my health right now” is a complete sentence.)
Months 3–12 (maintenance): By now, many patients either (a) have found a dose and routine they can tolerate or
(b) have decided it’s not for them. For those who continue, the experience often shifts from “symptom management” to “habit building.”
The medication can make it easier to stick with a lower-calorie, heart-healthy patternmore vegetables, lean proteins, fewer ultra-processed
snacksbecause cravings aren’t as loud. Some people report improved energy as weight comes down, which makes walking or strength training
feel more doable. Others need intentional support to exercise, because eating less doesn’t automatically create a love affair with the treadmill.
The heart-health mindset: People with prior heart attack or stroke often find the most motivating part isn’t the scale.
It’s the idea of reducing the chance of “another event.” Many describe a mental shift: medication becomes part of a long-term prevention strategy,
similar to statins or blood pressure meds. That can also bring up practical emotionsstress about cost, fear of side effects, frustration with
supply issues, or disappointment if weight loss slows. The most resilient approach is to track more than pounds: blood pressure, waist size,
stamina, lab trends, and how consistently you can maintain heart-healthy routines.
Bottom line: Wegovy can be a powerful tool, but it’s rarely a “take shot, become superhero” experience. It’s more like:
take shot, adjust habits, manage side effects, keep showing upand let the small, steady wins add up.
Conclusion
Wegovy’s 20% reduction in major cardiovascular events is a meaningful development for adults with established cardiovascular disease and
overweight or obesity. The SELECT trial suggests semaglutide can reduce heart attack, stroke, and cardiovascular death as a composite outcome,
while also supporting weight loss, modest blood pressure improvement, and fewer transitions into diabetes.
The key is using it thoughtfully: in the right population, alongside lifestyle changes and standard cardiac prevention therapies, with clear-eyed
attention to side effects and safety warnings. If you’re a candidate, the best next step is a clinician conversation grounded in your personal risk,
your medical history, and your ability to stay on treatment long enough to earn the benefit.