Table of Contents >> Show >> Hide
- What is gout in the big toe?
- How to identify gout in the big toe
- Why gout often attacks the big toe
- What causes gout in the big toe?
- How doctors diagnose gout in the big toe
- Treatment for gout in the big toe
- Long-term treatment to prevent future gout attacks
- Lifestyle changes that help with gout
- When to see a doctor right away
- Can gout in the big toe become chronic?
- Experiences people commonly have with gout in the big toe
- Final thoughts
If your big toe suddenly feels like it picked a fight with a hammer at 2 a.m., gout may be the uninvited guest. This type of inflammatory arthritis is famous for striking the joint at the base of the big toe with dramatic flair: sharp pain, redness, swelling, heat, and a level of tenderness that makes even a bedsheet feel rude.
The good news is that gout in the big toe is highly treatable. The better news is that once you know how to identify it, what causes it, and how treatment works, you can stop guessing and start managing it like a pro. In this guide, we’ll break down the symptoms, risk factors, diagnosis, and treatment options for gout in the big toe in plain American English, without turning the whole thing into a medical word salad.
What is gout in the big toe?
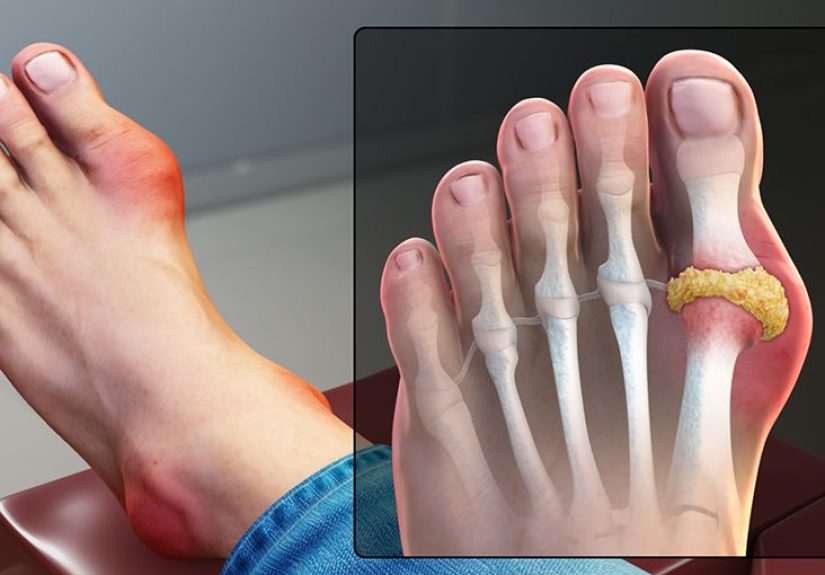
Gout is a form of inflammatory arthritis caused by a buildup of uric acid in the body. When uric acid levels stay too high over time, tiny needle-shaped urate crystals can form in and around a joint. The immune system reacts to those crystals like they just insulted its family, and the result is a painful gout flare.
When this happens in the joint at the base of the big toe, it is often called podagra. That joint is one of the most common places for a first gout attack. It is also one of the least convenient places to have one, since walking, standing, shoes, and basic dignity all depend on it.
How to identify gout in the big toe
Classic gout symptoms
Big-toe gout usually does not sneak in politely. It tends to arrive fast and loud. Many people describe waking up with pain that was not there when they went to sleep, or feeling a mild ache that turns into full-on misery within hours.
Common signs of gout in the big toe include:
- Sudden, intense pain in the joint at the base of the big toe
- Swelling that makes the toe look puffy or enlarged
- Red or purplish skin over the joint
- Warmth or heat in the area
- Extreme tenderness, even from light touch or a bedsheet
- Difficulty walking, standing, or wearing shoes
A flare often peaks within the first 12 to 24 hours. Without treatment, symptoms may gradually improve over several days to a couple of weeks. That “it got better on its own” part is one reason gout gets ignored early. Then it comes back later, usually with worse manners.
What gout pain feels like
Not every sore toe is gout, but gout has a personality. People often describe it as throbbing, burning, stabbing, or crushing pain. The toe may feel too painful to bend. Shoes can feel impossible. Walking across the room may suddenly look like an Olympic event.
Signs it may be something else
Plenty of conditions can cause big-toe pain, so it is smart not to self-diagnose based on one bad morning. Big-toe gout can sometimes be confused with:
- A bunion
- Osteoarthritis
- A toe fracture or sprain
- Cellulitis or another infection
- Septic arthritis
- Calcium crystal arthritis, sometimes called pseudogout
- An ingrown toenail if the pain is closer to the nail area
If the toe is very red, you have a fever, or the pain is severe and new, do not assume it is “just gout.” An infected joint is a medical emergency and can look similar at first.
Why gout often attacks the big toe
The big toe is a favorite target for a few reasons. First, urate crystals are more likely to form in cooler parts of the body, and toes are farther from your warm core. Second, the big toe joint takes a beating from walking, standing, and small everyday injuries. That repeated stress may help trigger inflammation when crystals are already present.
In other words, the big toe is the perfect storm: a hardworking joint, a little cooler than other body parts, and constantly asked to cooperate with your entire body weight. Rude, but medically consistent.
What causes gout in the big toe?
The root cause of gout is hyperuricemia, which means higher-than-normal uric acid levels in the blood. Uric acid is made when the body breaks down purines, substances found naturally in your body and in certain foods and drinks.
Normally, uric acid dissolves in the blood, travels to the kidneys, and leaves through urine. But if your body makes too much uric acid or your kidneys do not remove enough of it, levels can rise. That creates the conditions for crystal formation and painful flares.
Risk factors for gout
Several factors make gout more likely:
- Sex and age: Gout is more common in men, though women can develop it too, especially after menopause.
- Family history: If gout runs in your family, your odds may be higher.
- Kidney disease: Reduced kidney function makes it harder to clear uric acid.
- High blood pressure and heart disease: These often travel with gout.
- Obesity or excess body weight: This can increase uric acid production and lower excretion.
- Type 2 diabetes or metabolic syndrome: These conditions are linked to higher gout risk.
- Diet: Frequent intake of purine-rich foods can contribute.
- Alcohol: Beer and liquor are especially common culprits.
- Sugary drinks: Beverages sweetened with fructose may raise uric acid levels.
- Certain medicines: Diuretics, low-dose aspirin, and some other medications may increase uric acid.
Foods and drinks that may trigger a flare
Diet does not cause every case of gout, and one cheeseburger does not automatically doom your toe. Still, certain foods and drinks can raise uric acid or trigger flares in people who are already prone to gout.
Common dietary triggers include:
- Organ meats such as liver
- Red meat in large amounts
- Shellfish and some seafood, including anchovies, sardines, mussels, and scallops
- Beer and hard liquor
- Sugary sodas and drinks sweetened with high-fructose corn syrup
Diet matters, but it is only one piece of the puzzle. Many people with gout also need medication to truly control uric acid and prevent future attacks.
How doctors diagnose gout in the big toe
Medical history and physical exam
A clinician will usually start by asking when the pain began, how quickly it came on, whether you have had similar attacks before, what medicines you take, and whether you have kidney problems or other related conditions. They will also examine the toe for swelling, redness, warmth, and range of motion.
Blood tests
A blood test may be used to check your uric acid level. That can help, but it is not a perfect yes-or-no answer. Some people can have normal uric acid during a flare, while others may have high uric acid without having gout symptoms. So a blood test is useful, but it is not the whole story.
Joint fluid testing
The most definitive way to confirm gout is to remove a small sample of fluid from the affected joint and look for urate crystals under a microscope. This is called joint aspiration or arthrocentesis. It is especially helpful when the diagnosis is uncertain or when a doctor needs to rule out an infection.
Imaging tests
Ultrasound or special CT imaging may also help detect urate crystal buildup. Imaging can be useful when symptoms are confusing, attacks are recurring, or the doctor suspects long-term damage or crystal deposits called tophi.
Treatment for gout in the big toe
Gout treatment usually has two goals. The first is to calm the current flare. The second is to prevent future attacks by lowering uric acid over time. Those are related goals, but they are not the same thing.
Treating an acute gout flare
Common treatments for a painful flare include:
- NSAIDs: Prescription or over-the-counter anti-inflammatory drugs may reduce pain and swelling, depending on your health history.
- Colchicine: This medicine works best when started early in a flare.
- Corticosteroids: These may be given by mouth or sometimes injected into the joint when appropriate.
The right choice depends on your other medical conditions, kidney function, stomach history, current medications, and how severe the flare is. This is not a great time for freestyle medicine cabinet experiments.
Home care during a flare
Along with prescribed treatment, these steps may help ease discomfort:
- Rest the foot and avoid unnecessary walking
- Elevate the foot when sitting or lying down
- Apply ice wrapped in a towel for short periods
- Stay well hydrated unless your clinician has told you to limit fluids
- Avoid alcohol during the flare
- Do not squeeze into tight shoes just to prove a point
Long-term treatment to prevent future gout attacks
Urate-lowering medications
If you have repeated gout attacks, tophi, kidney stones, or ongoing high uric acid problems, your doctor may recommend a urate-lowering medication. These treatments address the root issue by reducing uric acid levels over time.
Common long-term options include:
- Allopurinol: Often a first-line medicine for lowering uric acid
- Febuxostat: Another option for some patients
- Probenecid: Sometimes used to help the body remove more uric acid
- Pegloticase: Reserved for severe or difficult-to-treat gout in select cases
These medicines do not usually provide instant pain relief during a flare. Their job is to lower uric acid steadily and reduce the chance of future attacks. That is why some people get frustrated and think the medicine “isn’t doing anything,” when in fact it is doing the slow, boring, extremely valuable work behind the scenes.
Doctors often aim for a serum urate target low enough to keep crystals from forming and to help existing deposits dissolve over time. Many patients are treated to a uric acid goal below 6 mg/dL, though targets can vary in more severe disease.
Why flares can happen when treatment starts
Starting a urate-lowering medicine can temporarily trigger flares at first because crystal deposits begin shifting as uric acid levels change. That sounds unfair because it is. To reduce the chance of this happening, doctors may prescribe low-dose colchicine, an NSAID, or another anti-inflammatory medication for a period of time when starting long-term treatment.
Lifestyle changes that help with gout
Medication often does the heavy lifting, but lifestyle changes can still make a real difference. Think of them as backup dancers that quietly make the whole show better.
Helpful habits for gout prevention
- Maintain a healthy body weight if recommended by your clinician
- Drink enough water
- Limit beer and liquor
- Cut back on sugary sodas and sweetened drinks
- Moderate portions of red meat and high-purine seafood
- Follow treatment for blood pressure, kidney disease, diabetes, and other related conditions
- Take gout medicines exactly as prescribed, even when you feel fine
Some people also benefit from a lower-purine eating pattern that emphasizes vegetables, fruit, whole grains, low-fat dairy, and balanced protein choices. No diet can guarantee zero flares, but an overall healthy pattern can support medication and reduce triggers.
When to see a doctor right away
Make prompt medical contact if:
- You have sudden, severe big-toe pain and have never been diagnosed with gout
- You have fever, chills, or feel generally ill
- The joint is extremely red, hot, and rapidly worsening
- You cannot bear weight on the foot
- Your symptoms are not improving with treatment
- You are having frequent attacks or developing lumps under the skin that may be tophi
An untreated infection, severe inflammation, or recurrent uncontrolled gout can lead to bigger problems than one angry toe.
Can gout in the big toe become chronic?
Yes. If uric acid stays high and gout is left untreated, flares may become more frequent, affect more joints, and lead to long-term complications. Over time, some people develop tophi, which are firm deposits of urate crystals under the skin. Chronic gout can also contribute to joint damage and disability.
That is why the goal is not only to survive one flare but to prevent the sequel, the reboot, and the unnecessary spin-off series.
Experiences people commonly have with gout in the big toe
Many people’s first experience with gout in the big toe is confusion. They go to bed feeling mostly fine and wake up convinced they somehow injured the toe in their sleep. The pain can seem wildly disproportionate to what the toe looks like at first. A person may think, “It’s just a sore toe,” and then discover that standing up feels like stepping on broken glass. That mismatch between appearance and pain is one reason gout surprises so many people.
Another common experience is mistaking the flare for something mechanical, like a bunion, bad shoes, or overdoing it at the gym. Because the big toe is such a busy joint, people often assume they simply strained it. Some try new shoes, foot pads, or rest for a day or two before realizing the redness, heat, and throbbing are not typical wear-and-tear symptoms. By then, even the pressure of a sock can feel unbearable.
People also often notice patterns only after several flares. For some, the attack shows up after a weekend of heavier eating and drinking. For others, it follows dehydration, illness, travel, a medication change, or a period of stress. The common thread is that gout tends to reveal itself in episodes. A person may have one brutal flare, recover, and then ignore it for months. When it happens again, the pattern starts to become obvious.
There is also the emotional side of the experience, which does not get enough attention. Gout pain can be intense enough to interrupt sleep, cancel plans, and make normal routines feel ridiculous. Walking to the bathroom becomes strategic. Stairs become enemies. Shoes become negotiation tools. Some people feel embarrassed because gout has an old-fashioned reputation, as if it only happens to kings, pirates, and people who apparently dine on steak by candlelight every evening. In reality, gout is a common medical condition with metabolic, kidney, genetic, and lifestyle factors all mixed together.
One of the most important experiences people report after proper treatment is relief at finally understanding what is happening. Once a clinician explains the difference between treating a flare and preventing the next one, gout starts to make more sense. Patients often say the turning point is not just getting pain relief, but learning that long-term uric acid control matters even when the toe feels normal. That shift in mindset can be huge.
Many people also learn that small daily habits matter more than dramatic one-week efforts. Staying hydrated, being careful with alcohol, taking prescribed medication consistently, and following up on uric acid levels usually works better than panic-searching the internet during a midnight flare. In real life, gout management is often less about one magical food and more about steady, boring, effective routines. Not glamorous, but neither is limping around your kitchen because your toe declared a state of emergency.
Final thoughts
Gout in the big toe is one of the most recognizable forms of arthritis, but it still gets misunderstood. The pain is real, the cause is specific, and the treatment can be very effective when matched to the person. If your big toe becomes suddenly swollen, red, hot, and incredibly painful, especially overnight, gout should be on the list of possibilities.
The smartest move is to get an accurate diagnosis, treat the flare promptly, and talk with a healthcare professional about long-term prevention if attacks keep happening. With the right plan, your toe can go back to doing what it was meant to do: helping you walk around instead of starring in a one-joint disaster movie.





