Table of Contents >> Show >> Hide
Introduction
Tuberculosis (TB) is a serious infectious disease that primarily affects the lungs but can spread to other parts of the body. With millions of cases diagnosed annually worldwide, understanding how tuberculosis is diagnosed through screenings and tests is crucial in controlling its spread. The diagnosis of TB involves several steps, starting with identifying symptoms and moving through a series of tests to confirm the infection. In this article, we’ll dive into the methods healthcare professionals use to diagnose TB, and why early detection is vital in preventing complications.
What is Tuberculosis?
Tuberculosis is a disease caused by the bacterium Mycobacterium tuberculosis. It typically spreads through the air when an infected person coughs, sneezes, or talks, making it highly contagious. TB can affect different parts of the body, but it most commonly targets the lungs. Though it can be treated with antibiotics, if left untreated, it can lead to severe health complications or even death.
Initial Screening for Tuberculosis
The first step in diagnosing tuberculosis is usually a screening process, which aims to identify individuals who may be at higher risk of the disease. This often includes both a medical history review and a physical examination, during which doctors look for common TB symptoms, such as persistent cough, unexplained weight loss, night sweats, fever, and fatigue. If a person shows signs of TB, further testing is conducted.
1. The Tuberculin Skin Test (TST)
One of the most common methods used for initial screening is the Tuberculin Skin Test (TST), also known as the Mantoux test. This test involves injecting a small amount of purified protein derivative (PPD) from the tuberculosis bacteria just under the skin on the forearm. After 48 to 72 hours, the healthcare provider checks the injection site for any reaction. A raised, hard area at the site of injection indicates that the person has been exposed to the tuberculosis bacteria.
The TST doesn’t confirm an active TB infection, but it helps determine whether someone has been exposed to the TB bacteria at some point in their life. A positive result might indicate latent TB infection (LTBI), where the bacteria are present in the body but are not causing symptoms or being spread to others.
2. The Interferon-Gamma Release Assays (IGRAs)
Another method used for TB screening is the Interferon-Gamma Release Assay (IGRA), a blood test that measures the immune response to TB bacteria. Unlike the TST, IGRAs do not require a follow-up visit to check for a skin reaction. IGRAs are particularly useful for individuals who have received the BCG vaccine or those who may not have a clear reaction to the TST.
The results of an IGRA are usually available within a few hours, providing a more convenient option for testing, especially in high-risk populations.
Diagnostic Tests for Active Tuberculosis
If initial screening tests suggest the possibility of tuberculosis infection, further diagnostic tests are conducted to confirm whether the person has an active TB infection. These tests are crucial in determining the appropriate course of treatment and ensuring the person does not spread the disease to others.
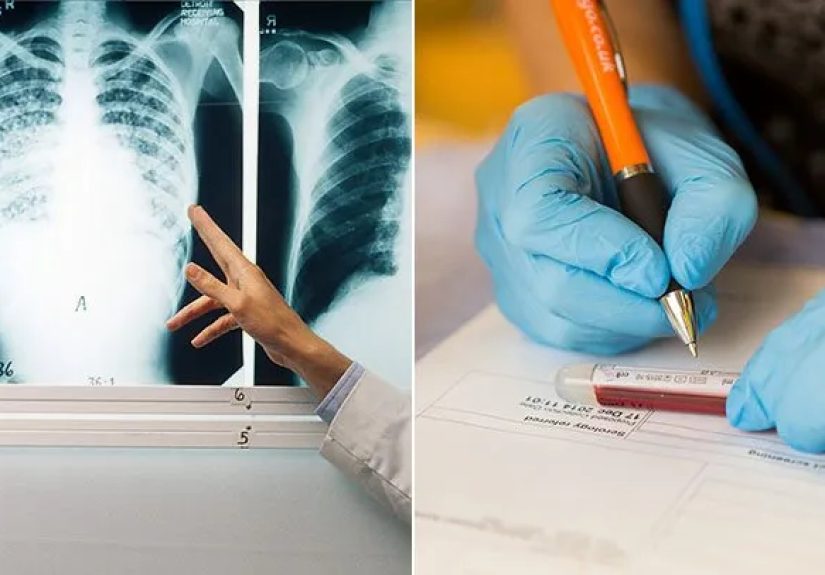
3. Chest X-Ray
The chest X-ray is one of the most widely used tests to detect active tuberculosis. It helps to visualize any abnormalities in the lungs, such as lesions, cavities, or fluid buildup, that might suggest an active infection. If the X-ray shows signs consistent with TB, additional tests are often ordered to confirm the diagnosis.
4. Sputum Smear Microscopy
Another key test is the sputum smear microscopy, which involves examining a sample of sputum (mucus coughed up from the lungs) under a microscope. The presence of acid-fast bacilli (AFB), which are TB bacteria, in the sputum sample can confirm an active TB infection. This test is particularly important for individuals with respiratory symptoms like coughing or shortness of breath.
In addition to diagnosing TB, sputum smear microscopy can help determine the severity of the disease. In areas with limited resources, this is often one of the first tests conducted for suspected TB cases.
5. Sputum Culture
A sputum culture is another critical test used to confirm active TB. Unlike the smear test, which looks for bacteria directly, a culture allows for the growth of bacteria from the sputum sample. Culturing the bacteria can take several weeks but provides definitive proof of infection. It also helps to determine whether the bacteria are resistant to the commonly used drugs, which is crucial for treatment planning.
6. Molecular Tests (PCR Tests)
Polymerase chain reaction (PCR) tests are molecular tests that detect the DNA of the tuberculosis bacteria in sputum or other samples. PCR tests are faster than sputum cultures and are highly sensitive, making them valuable for diagnosing TB more quickly, especially in people with HIV or those who may have a weakened immune system. They are also essential for detecting drug-resistant strains of tuberculosis, which can significantly impact treatment decisions.
Diagnosis of Drug-Resistant Tuberculosis
Drug-resistant tuberculosis (DR-TB) is a growing concern worldwide. This occurs when the TB bacteria become resistant to the drugs most commonly used to treat the disease, such as isoniazid and rifampin. To diagnose DR-TB, healthcare providers typically use more advanced tests such as molecular tests and sputum culture for drug resistance testing. If drug resistance is detected, a more tailored treatment regimen is prescribed, which may involve second-line TB drugs.
Additional Tests for Extrapulmonary Tuberculosis
While TB usually affects the lungs, it can also spread to other parts of the body, including the kidneys, spine, brain, and lymph nodes. This is known as extrapulmonary tuberculosis. Diagnosis of extrapulmonary TB often involves biopsies or fluid collection from the affected site, followed by culture and molecular tests. Chest X-rays might also be used to rule out pulmonary TB in individuals with symptoms of extrapulmonary TB.
Conclusion
Early diagnosis of tuberculosis is essential for preventing its spread and ensuring that individuals receive timely and appropriate treatment. The diagnostic process for TB involves several steps, including initial screenings with the tuberculin skin test or interferon-gamma release assays, followed by confirmatory tests like chest X-rays, sputum smears, cultures, and molecular tests. As TB can be a life-threatening disease, understanding how it is diagnosed helps individuals and healthcare providers take proactive steps toward detection and treatment.
Experiences Related to Diagnosing Tuberculosis
While the methods used to diagnose tuberculosis are relatively straightforward, the process can sometimes feel overwhelming for patients. When I first visited the clinic for a TB screening, I was nervous. The thought of undergoing a skin test made me anxious, not because I feared the results, but because of the potential wait time. However, the nurse who administered the test reassured me, explaining that the process was quick, and that follow-up was simple. The skin test result came back negative, but I still underwent a chest X-ray to rule out any lung involvement.
One of my friends, on the other hand, had a positive tuberculin skin test result, which led to a more detailed investigation. She was relieved to learn that the subsequent sputum smear and culture came back negative, ruling out active TB. She was, however, diagnosed with latent TB and put on a course of preventive antibiotics. This experience highlighted the importance of screening even for those who do not show obvious symptoms.
As we move towards more advanced technologies, such as PCR and molecular testing, the process of diagnosing TB is becoming faster and more accurate. I’ve heard that PCR tests have revolutionized the diagnosis of drug-resistant TB, allowing doctors to start the right treatment much earlier, reducing the chances of complications. While not everyone has access to the latest technology, these advancements are a step in the right direction in the fight against tuberculosis.