Table of Contents >> Show >> Hide
- What Is the Lachman Test?
- Why the ACL Matters (and Why Your Knee Cares So Much)
- When Is the Lachman Test Used?
- How the Lachman Test Is Performed (Step-by-Step, Patient-Friendly)
- What Is a “Positive” Lachman Test?
- Lachman Test Grading: What Grade 1, 2, and 3 Really Mean
- How Accurate Is the Lachman Test?
- Lachman vs Anterior Drawer vs Pivot Shift: What’s the Difference?
- What Happens After a Positive Lachman Test?
- Can You Do the Lachman Test on Yourself?
- Common Questions (Because Knees Make People Curious)
- Key Takeaways
- Real-World Experiences (Common Stories Patients and Clinicians Recognize)
- Conclusion
Quick note: This article is for general education, not a diagnosis. If your knee is swollen, unstable, or you can’t bear weight, get evaluated by a qualified clinician.
What Is the Lachman Test?
The Lachman test is a hands-on knee exam used to check the integrity of the anterior cruciate ligament (ACL)the ligament that helps keep your shinbone (tibia) from sliding too far forward under your thighbone (femur), and also helps control rotation. Think of the ACL as a sturdy “seatbelt” inside the knee: it doesn’t stop all motion, but it keeps motion from becoming a chaotic joyride.
Clinicians often reach for the Lachman test when someone has symptoms that suggest an ACL injuryespecially after a twisting injury, an awkward landing, or a sudden change of direction. It’s commonly used on the sidelines, in urgent care, in sports medicine clinics, and in orthopedic offices.
Why the ACL Matters (and Why Your Knee Cares So Much)
The ACL runs diagonally inside the knee and primarily limits anterior translation (forward movement) of the tibia relative to the femur. It also contributes to rotational stability. When the ACL is torn or significantly stretched, the knee may feel:
- Unstable (a “giving way” sensation)
- Swollen, often within hours after injury
- Painful, especially during pivoting or cutting movements
- Less trustworthylike walking on a floorboard that squeaks for a reason
When Is the Lachman Test Used?
The Lachman test is typically used when there’s suspicion of an ACL injury based on:
- A non-contact pivot or twist (soccer, basketball, football, skiing)
- A pop felt or heard at the time of injury
- Rapid swelling (possible bleeding into the joint)
- Instability when trying to return to activity
- A knee injury where the clinician wants to compare multiple stability tests
It’s also used in follow-upssuch as after ACL reconstructionto assess stability over time.
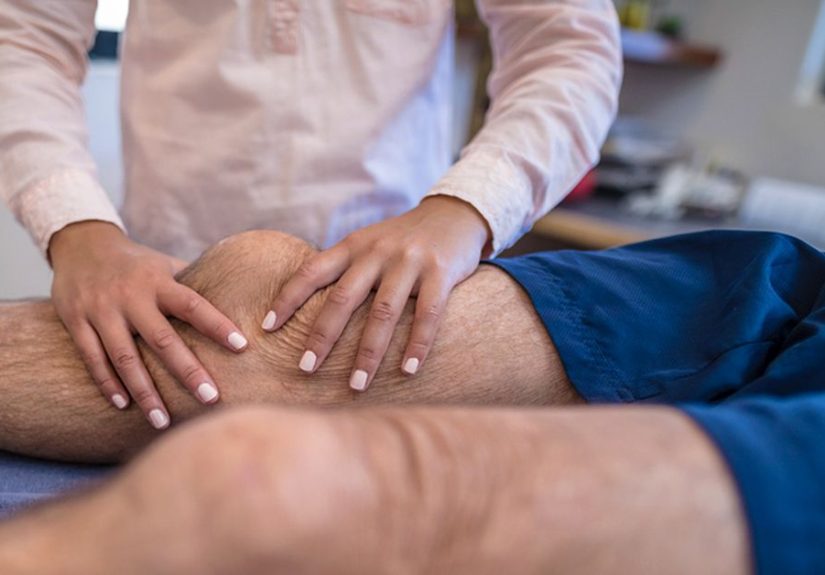
How the Lachman Test Is Performed (Step-by-Step, Patient-Friendly)
Clinicians perform the Lachman test with you lying on your back (supine). The key is a slightly bent kneeusually around 20–30 degrees of flexion. That angle helps “isolate” the ACL more than some other positions.
What the examiner does
- Positions your knee in slight flexion (about 20–30°).
- Stabilizes the femur with one hand (so the thighbone doesn’t move).
- Grasps the upper tibia with the other hand.
- Applies an anterior pull to the tibia while keeping the femur steady.
- Assesses two things:
- How far the tibia moves compared with the uninjured knee
- The “endpoint” feelwhether motion stops with a firm check (good) or slides without a clear stop (concerning)
What you might feel
Many people feel pressure or mild discomfort, especially if the knee is swollen. The test should not be a pain contest. If pain or muscle guarding makes the exam unreliable, clinicians may re-check later, manage swelling first, or use imaging and other tests to confirm the diagnosis.
What Is a “Positive” Lachman Test?
A positive Lachman test generally means the tibia moves forward more than expected compared with the other knee, and/or the examiner feels a soft or absent endpoint instead of a firm stop.
Because everyone’s baseline looseness differs, clinicians usually compare the injured knee to the uninjured side. A little motion can be normal; a lot of motion with a “mushy” endpoint is the part that raises eyebrows (the medically appropriate kind, not the judgmental kind).
Lachman Test Grading: What Grade 1, 2, and 3 Really Mean
Grading systems vary a bit by clinic and training, but many clinicians describe ACL laxity on a scale from Grade 1 (mild) to Grade 3 (severe), often using side-to-side differences in millimeters.
A commonly used grading framework
- Grade 1 (mild): About 0–5 mm more anterior translation than the uninjured side.
- Grade 2 (moderate): About 6–10 mm more translation.
- Grade 3 (severe): About 11–15 mm more translation.
Endpoint grading: “A” vs “B” (why you might see “2B” or “3B”)
Some clinicians add endpoint quality to the grade:
- A endpoint: firm/hard endpoint (motion stops clearly)
- B endpoint: soft/absent endpoint (no clear stop)
So, a “3B Lachman” typically suggests a lot of translation and a poor endpointoften consistent with a significant ACL disruption. The grade helps communicate severity quickly, especially when planning imaging, referrals, and treatment.
How Accurate Is the Lachman Test?
In clinical practice, the Lachman test is widely considered one of the best physical exam maneuvers for suspected ACL tearsparticularly in the acute setting. That said, accuracy depends on factors like examiner technique, swelling, pain, and whether the patient can relax their muscles.
Why accuracy can change
- Swelling/hemarthrosis: Fluid in the joint can make movement painful and trigger guarding.
- Hamstring guarding: Tight hamstrings can “fake stability” by resisting tibial movement.
- Time since injury: In the first hours, swelling and pain may interfere; later, stiffness can also complicate the exam.
- Skill and hand placement: Small technique differences can change what the examiner feels.
Lachman vs Anterior Drawer vs Pivot Shift: What’s the Difference?
These tests often travel in a group because each tells a slightly different part of the ACL story.
Lachman test
- Knee flexed ~20–30°
- Focuses on anterior tibial translation and endpoint quality
- Often easier to perform in acute injuries than some alternatives
Anterior drawer test
- Knee flexed ~90°
- Also checks anterior tibial translation
- Can be affected more by hamstring guarding
Pivot shift test
- Assesses rotational instability (a classic feature of ACL deficiency)
- Often very convincing when positive
- Can be hard to do in the acute setting due to pain/guarding
Bottom line: A thorough knee evaluation often uses multiple maneuvers, not just one. Clinicians also assess other ligaments and the meniscus because ACL injuries can come with “bonus damage” nobody ordered.
What Happens After a Positive Lachman Test?
A positive Lachman test is not the finish lineit’s a big signpost that says, “We should look closer.” Next steps commonly include:
1) History + full knee exam
Clinicians review the mechanism of injury, swelling timing, functional limits, and perform additional tests for other ligaments and meniscus.
2) Imaging (often)
- X-ray: Can rule out fractures or avulsion injuries and assess bony alignment.
- MRI: Commonly used to confirm ACL damage and identify meniscus/cartilage injuries.
3) Treatment planning
Management depends on your age, sport/activity goals, associated injuries, and knee stability. Options may include:
- Rehab-focused care: Strengthening, neuromuscular training, swelling control, and return-to-activity planning.
- Bracing: Sometimes used for comfort or stability during certain phases.
- Surgical consultation: Often considered for athletes in pivoting sports, those with significant instability, or those with certain associated injuries.
Can You Do the Lachman Test on Yourself?
Realistically? Not reliably. The Lachman test depends on stabilizing the femur while translating the tibia and interpreting subtle differences in endpoint feel. Self-testing often turns into “I pulled something and now I’m anxious,” which is not a medical plan.
If you suspect an ACL injuryespecially with swelling, a pop, or instabilityseek professional evaluation. Early assessment can help prevent additional injury and guide the right next steps.
Common Questions (Because Knees Make People Curious)
Does a positive Lachman test always mean a complete ACL tear?
Not always. It suggests abnormal laxity consistent with ACL injury, but severity can vary. Partial tears, patient anatomy, and other ligament issues can influence findings. Imaging and a full exam help clarify what’s going on.
Can other injuries cause a “false positive” Lachman?
Yes. Certain patterns of knee injuryincluding issues involving other ligamentscan complicate interpretation. That’s why clinicians check multiple structures, not just the ACL.
Why compare to the other knee?
Because “normal” laxity differs from person to person. Some people are naturally more flexible, and comparing sides helps identify what’s abnormal for you.
Is the Lachman test safe?
When performed correctly by a trained clinician, it’s considered safe. If there’s suspicion of fracture, severe pain, or other red flags, clinicians adjust the exam and use imaging as needed.
Key Takeaways
- The Lachman test is a core physical exam maneuver for suspected ACL injury.
- A positive test usually means increased forward tibial movement and/or a soft endpoint compared to the other knee.
- Grading commonly describes severity (often by side-to-side translation in mm) and endpoint quality.
- Results are strongest when interpreted as part of a full knee evaluation, often with imaging like MRI.
Real-World Experiences (Common Stories Patients and Clinicians Recognize)
Important note: The experiences below are composite, real-world-style scenarios based on commonly reported patternsnot personal stories from the author and not a substitute for medical care.
1) “I heard a pop… then my knee blew up like a balloon.”
A classic ACL story starts with a quick pivotbasketball defense, soccer cut, a ski turn that caught an edge. Many people describe a pop, immediate instability, and swelling that ramps up within hours. In clinic, the challenge is that the knee is often tender and guarded. When the clinician attempts the Lachman test, the patient’s hamstrings may tense automatically (your body’s version of “nope”). A careful examiner may first focus on comfort: supporting the leg, using gentle technique, and comparing the uninjured side to set a baseline. Sometimes the exam is repeated after swelling and pain are better controlled, because a relaxed knee tells the truth more easily.
2) The “weekend warrior” who feels fine… until the next pivot
Another common experience: someone rests for a week or two, the swelling goes down, walking feels okay, and they think they escaped serious damage. Then they try a quick turnmaybe stepping off a curb while carrying groceries or returning to a casual gameand the knee gives way again. In these cases, the Lachman test may be easier to interpret because pain is lower, but instability is clearer. Patients often say the weird part isn’t the painit’s the lack of trust. They’ll describe avoiding stairs, hesitating on uneven ground, or feeling like the knee might “slide” at the wrong moment.
3) “My report says ‘2B Lachman.’ What does that even mean?”
Seeing grades and letters can feel like your knee got a report card you didn’t study for. Clinicians use grading to communicate severity quickly. A “2” suggests moderate increased translation; a “B” endpoint suggests the stop at the end of motion feels soft or absent. Patients often find it helpful when the clinician translates the jargon into function: “Your knee is moving more than it should, and it doesn’t have that firm check that an intact ACL provides.” That explanation connects the exam finding to why pivoting or sudden stops feel unstable.
4) The post-op follow-up: “It feels stable, but I’m scared to move fast.”
After ACL reconstruction, many people are surprised by how much the mental side matters. Even when strength is improving and the Lachman test feels stable on exam, confidence may lag behind. Patients often describe returning to running before they feel ready to cut or pivot. Good rehab programs treat this as normal: they build stability, control, and gradual exposure to sport-like movements. In other words, it’s not just “Is the ligament stable?” but also “Does your brain believe the knee is stable?”
5) The teen athlete and the family meeting
In younger athletes, an injury that threatens sports participation can feel hugefor the athlete and their family. Clinicians often use the Lachman test as one piece of a bigger conversation: what’s the injury, what does imaging show, what are the options, and what timeline makes sense. Families usually want clarity: “Is it torn? Do we need surgery? When can they return?” The most reassuring visits are the ones that combine a clear explanation of the exam (including Lachman grading) with a realistic plan: manage swelling, confirm injury details, protect the knee from giving-way episodes, and map out rehab and return-to-play criteria step by step.
If there’s one theme across these experiences, it’s this: the Lachman test isn’t just a “gotcha” maneuver. It’s a structured way to understand knee stabilityso the next decisions (imaging, rehab, sport modifications, and sometimes surgery) are based on evidence, not vibes.
Conclusion
The Lachman test is a staple in knee exams for a reason: it helps clinicians quickly assess ACL integrity by evaluating forward tibial movement and endpoint quality. Grading adds useful detail about severity, and a positive result often leads to further evaluationcommonly including MRIto confirm the diagnosis and check for associated injuries. If your knee feels unstable, swells quickly after injury, or “gives way,” a professional evaluation can help you protect the joint and plan the safest path back to activity.







