Table of Contents >> Show >> Hide
- What Hand Psoriasis Looks Like (and Why Pictures Help)
- Gentle Cleansing: The First “Picture” in Your Hand-Care Routine
- Moisturizing Like a Pro: Turning Dry Plaques into Softer Skin
- Gloves, Triggers, and Everyday Protection
- Working With Your Dermatologist on a Treatment Plan
- Seeing the Bigger Picture: Triggers and Lifestyle Factors
- When to Call Your Dermatologist (or Primary Care Clinician)
- Real-Life Experiences: What Managing Hand Psoriasis Feels Like Day to Day
- Conclusion: Turning Your Hand Photos into a Plan
If you have psoriasis on your hands, you probably already have your own mental photo gallery:
the morning your knuckles looked like they were dusted with flour, the day your fingertips
cracked right before an important meeting, or the time someone asked, “Did you burn yourself?”
(No. No, you did not.)
While we can’t embed your real-life hand selfies here, we can walk through picture-style
tips for managing psoriasis on your hands. Think of this article as a guided slideshow:
each “slide” is a scene that shows you exactly what good hand care can look like in daily life.
We’ll break down what hand psoriasis often looks like, how to care for your skin gently,
how to use moisturizer and gloves strategically, and how to work with your dermatologist
on a treatment plan. We’ll also talk about lifestyle triggers and end with real-world,
experience-based tips to help you feel less alone and more in control.
What Hand Psoriasis Looks Like (and Why Pictures Help)
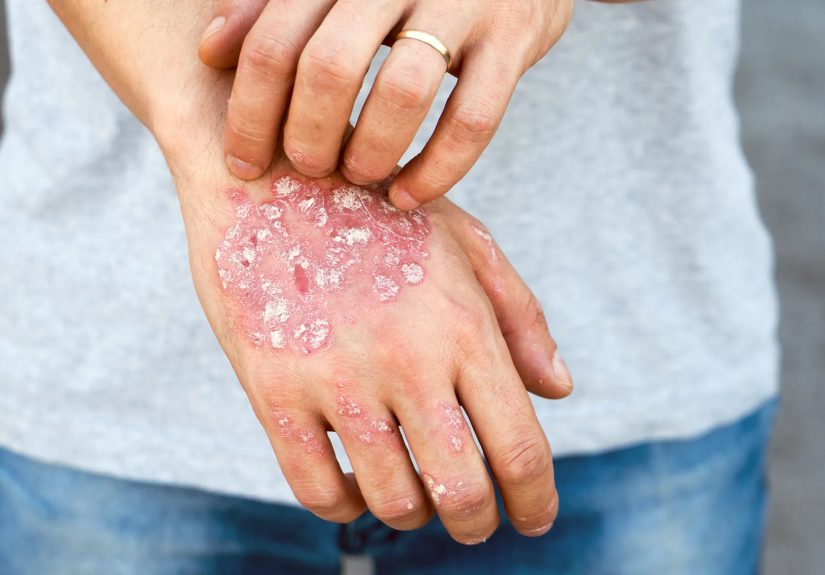
Psoriasis on your hands can show up in many ways. Some people see small, dry patches;
others develop thick plaques, painful cracks, or even changes in the nails. The appearance
can change week to week, which is why tracking it with photos can actually be helpful.
Common visual signs of psoriasis on your hands
-
Red or darker patches on the backs of the hands, knuckles, or palms,
often covered with silvery or whitish scale. -
Thickened, rough plaques that may feel raised or “stacked,”
especially on areas that rub against objects (like the base of your fingers). -
Cracks and fissures along the creases or fingertips that can sting,
bleed, or make simple tasks like buttoning a shirt painful. -
Itching or burning that makes you want to scratch, even though scratching
usually makes things worse. -
Nail changes such as pitting (tiny dents), discoloration, or thickening
if nail psoriasis is also involved.
Many people use hand photos to keep track of flares. A simple wrist-to-fingertip picture
taken every few weeks can show how well a new moisturizer, prescription cream, or habit
change is working. It can also give your dermatologist a clear before-and-after view of your skin.
Gentle Cleansing: The First “Picture” in Your Hand-Care Routine
Imagine a close-up shot of your hands at the sink. The water is lukewarm,
not hot enough to steam up your mirror. Next to the faucet is a pump bottle of
fragrance-free, gentle cleanser or emollient wash instead of a harsh, foaming soap.
That’s the kind of scene dermatologists like to see. Hot water and strong soaps
strip away natural oils and can worsen dryness and irritation. A gentle routine
helps maintain your skin barrier, which is already under stress from inflammation.
Step-by-step, picture-style hand-washing routine
- Turn on lukewarm water. Avoid very hot water that can dry and irritate skin.
-
Use a gentle cleanser or emollient wash. Look for labels like
“fragrance-free,” “for sensitive skin,” or “emollient-based.” Avoid gritty scrubs
and deodorant soaps. -
Wash softly, not aggressively. You’re cleaning the skin,
not trying to scrub the psoriasis away (unfortunately, it doesn’t work like that). - Rinse thoroughly. Leftover soap can be irritating.
- Pat dry with a soft towel. No vigorous rubbing. Think “blotting,” not “buffing.”
-
Immediately apply moisturizer. This is the crucial final frame:
moisturize while the skin is still slightly damp to seal in hydration.
Doing this consistently may feel repetitive, but over time it can change the “look”
of your hands from tight and flaky to calmer and more comfortable.
Moisturizing Like a Pro: Turning Dry Plaques into Softer Skin
If we could take a split-screen picture of psoriasis-friendly hand care,
one side would show dry, chalky patches after handwashing with no moisturizer.
The other side would show a glossy, slightly shiny finish from a thick cream or ointment.
Guess which side usually feels better.
Moisturizing isn’t just about comfort; it’s a core part of psoriasis management.
Emollients (moisturizing creams, lotions, ointments, and balms) help soften scale,
reduce itching, and support your skin’s barrier so it’s less reactive.
What to look for in a hand moisturizer for psoriasis
-
Thick texture: Creams and ointments are usually more effective
than very light lotions. - Fragrance-free and dye-free: Added fragrance and colorants can be irritating.
-
Barrier-supporting ingredients: Products with ceramides, petrolatum,
glycerin, or hyaluronic acid may help lock in moisture. -
“For sensitive or very dry skin” labeling: These are often
designed with fewer potential irritants.
How to use moisturizer (picture it step by step)
-
Apply several times a day. The classic moments: after every handwash,
before going out in cold weather, and right before bed. -
Use enough product. Don’t be shy. A pea-sized dab for each hand is a starting point;
you may need more if plaques are thick or extensive. -
Cover the entire hand. Backs of hands, palms (if affected),
between fingers, knuckles, and around the nails. -
Try “overnight glove therapy.” At night, apply a thick layer of ointment or cream,
then slip on soft cotton gloves. This can create a “mini spa” occlusion effect that boosts absorption
and helps reduce cracking by morning.
Over time, you may notice your “after” photos show less scaling, fewer deep fissures,
and a smoother overall texture. That doesn’t mean psoriasis is gone, but it often means
your skin barrier is happier.
Gloves, Triggers, and Everyday Protection
Picture a busy day: you’re washing dishes, cleaning the bathroom, opening boxes,
maybe doing a little yard work. In each of those scenes, your hands meet detergents,
hot water, rough cardboard, or cold air all of which can aggravate hand psoriasis.
Using gloves strategically
-
Household chores: Wear protective gloves when you’re using cleaning products,
doing dishes, or soaking your hands in water for a long time. -
Choose materials wisely: Many people do well with vinyl or nitrile gloves,
often layered over thin cotton gloves. Cotton helps absorb sweat and protects skin
from rubbing and irritation. -
Avoid latex if you’re sensitive: Some people have
latex allergy or irritation, which can worsen redness and itchiness. -
Cold weather scenes: In outdoor winter photos, your hands should be wearing
warm, breathable gloves to protect from dry, cold air.
Think of gloves as props in your daily “psoriasis movie”: they aren’t just accessories,
they’re part of your treatment-supporting toolkit.
Working With Your Dermatologist on a Treatment Plan
While skin care habits are important, psoriasis is an immune-mediated condition,
not just “dry skin.” That’s why partnering with a dermatologist is key
especially when psoriasis affects your hands, which you need for nearly everything.
Topical treatments you might see in your “medicine cabinet picture”
Your dermatologist may recommend or prescribe:
-
Topical corticosteroids: These anti-inflammatory creams or ointments
are commonly used to calm active plaques. Potency and schedule depend on where the psoriasis is
and how severe it is. -
Vitamin D analog creams: Often used along with steroids,
these help slow the overgrowth of skin cells. -
Calcineurin inhibitors: These non-steroid anti-inflammatory creams
can sometimes be used in sensitive areas or as a steroid-sparing option. -
Topical retinoids or salicylic acid products: These may help soften scale
and support the shedding of thick plaques when used under medical supervision.
For more extensive or stubborn hand psoriasis, your dermatologist may consider
light therapy (phototherapy) or systemic medications (such as pills or biologic injections).
These decisions are highly individualized, based on how much of your body is affected,
how your joints feel, and how psoriasis is impacting your daily life.
Important note: This article is for education, not a DIY prescription plan.
Always follow your clinician’s instructions and ask before adding new over-the-counter
products on top of prescribed medications.
Seeing the Bigger Picture: Triggers and Lifestyle Factors
If you lined up photos of your hands over several months, you might notice patterns:
flares after a stressful week, during cold, dry weather, or after trying a new scented soap
or lotion. These “background scenes” are just as important as the close-up shots of your skin.
Common psoriasis triggers that can show up in your hands
-
Stress: Emotional or physical stress is a well-known trigger.
Many people notice hand plaques worsening during big life changes, deadlines,
or when sleep is poor. -
Skin injury or irritation: Cuts, scrapes, friction,
or harsh chemicals can sometimes spark new plaques in that area (a phenomenon called the Koebner response). -
Dry air and cold weather: Low humidity and cold temperatures
can dehydrate skin and exaggerate scaling and cracking. -
Smoking and heavy alcohol use: These may worsen psoriasis overall
and interfere with some treatments. -
Dietary patterns in some people: While food isn’t the root cause,
some individuals notice that anti-inflammatory eating patterns (more fruits, vegetables,
whole grains, and healthy fats; fewer ultra-processed foods and added sugars)
make their skin feel better overall.
Keeping a simple “photo + notes” journal can help. Snap a quick picture of your hands,
then jot down what’s been going on: stress level, new products you used,
weather changes, or any big lifestyle shifts. Over time, you and your dermatologist
may spot trends that help you personalize your trigger management.
When to Call Your Dermatologist (or Primary Care Clinician)
Even with great self-care, psoriasis on your hands can sometimes get out of control.
Reach out to a professional if you notice:
- Sudden worsening of redness, swelling, or pain.
- Yellow crusting, warmth, or pus, which might suggest infection.
- Cracks so deep you can’t comfortably use your hands at work or home.
- New nail changes, joint pain, or stiffness that might signal psoriatic arthritis.
- No improvement despite using treatments as directed.
If you can, bring your photo gallery to the visit it’s like handing your clinician
a time-lapse video of your psoriasis, which can be incredibly helpful for choosing
the next steps in your treatment plan.
Real-Life Experiences: What Managing Hand Psoriasis Feels Like Day to Day
Reading about “emollients” and “barrier support” is one thing; living with psoriasis
on your hands is another. Here are experience-based snapshots that mirror what many
people go through and how they adapt.
“The sink strategy”
One common turning point goes like this: someone realizes their hands look
worst on days when they’re constantly washing caregiving, food prep,
bathroom cleaning, the works. The “before” picture is raw, tight skin by evening.
The “after” picture, once they change their routine, tells a different story.
They switch to a fragrance-free gentle cleanser, stash a mini tube of cream near the faucet,
and make a deal with themselves: no handwashing without moisturizing afterward.
At first it feels like extra work. But after a couple of weeks of consistent “wash + moisturize”
photos, those angry, chalky patches often look flatter and calmer.
Glove hacks that actually get used
Another real-life scene: a person buys three different kinds of gloves and uses… none of them.
Why? Because they’re uncomfortable, sweaty, or left in a drawer.
What tends to work better is simplifying the “glove wardrobe”:
one pair of thin cotton gloves for nighttime moisturizing, and one box of vinyl or nitrile gloves
for cleaning and dishwashing. The cotton pair lives on the nightstand.
The vinyl gloves live under the kitchen sink. That way, they show up in the right “frames”
of daily life without a scavenger hunt.
Learning the difference between “dry skin” and “it’s a flare”
Many people describe a moment where they realize not every change in their hands
is a full flare, and not every good day means psoriasis is gone.
The photos help here: looking back, they can see subtle warning signs
a bit more redness around the knuckles, more scale on one patch on the thumb
that tend to show up a few days before a big flare.
Once they recognize those “preview frames,” they can respond earlier:
more consistent moisturizing, avoiding known irritants, and checking in with their dermatologist
if it keeps progressing. Instead of feeling ambushed by a flare, they feel more like
they are “reading the script” in advance.
Emotional snapshots: embarrassment, pride, and everything in between
Psoriasis on your hands is not just a skin issue; it’s a social one.
People notice hands. You might catch yourself hiding them in pockets,
under sleeves, or behind coffee cups during conversations.
Some people find it empowering to take pictures on both “bad” and “good” days
not to judge themselves, but to track progress and remind themselves that flares are temporary.
Looking back, they can see how far they’ve come with a better skin-care routine
and a treatment plan that works for them.
Others share their photos in support groups or online communities,
where “before and after” shots aren’t about perfection; they’re about finding people
who understand what it’s like when twisting open a jar or shaking someone’s hand
suddenly becomes complicated.
Building your own “psoriasis-on-hands” toolkit
Over time, many people assemble a toolkit that shows up again and again in their daily “pictures”:
- A favorite thick, fragrance-free hand cream or ointment.
- Cotton gloves for overnight moisturizing sessions.
- Vinyl or nitrile gloves for cleaning and dishwashing.
- A gentle, non-drying hand cleanser.
- A small notebook or phone app to match photos with notes about flares and triggers.
- Regular follow-ups with a dermatologist who takes their hand symptoms seriously.
None of these tools is magic on its own, but together they can change the “feel”
and “look” of daily life with psoriasis on your hands. Instead of constantly reacting to flares,
you’re proactively shaping your own care story, frame by frame.
Conclusion: Turning Your Hand Photos into a Plan
Living with psoriasis on your hands can be frustrating, painful, and sometimes embarrassing.
But the pictures you take whether literal photos or just mental snapshots
can become powerful tools. They show you which habits help, which products irritate,
how stress shows up in your skin, and how your treatment plan is working over time.
Gentle cleansing, frequent moisturizing, smart use of gloves, attention to triggers,
and ongoing conversations with your dermatologist form the backbone of good hand care.
Add in your own experience, a sense of humor, and some patience, and those “before”
and “after” shots may start to look more hopeful.
Remember: this article is information, not a diagnosis or prescription.
Always work with a healthcare professional to create a treatment plan that fits your
specific type of psoriasis, your health history, and your lifestyle.
SEO Meta Information
to smart moisturizing and trigger management.
sapo:
Psoriasis on your hands can turn everyday tasks into painful, self-conscious moments
but clear, picture-style tips can help you reclaim some comfort and confidence.
In this in-depth guide, you’ll “walk through” what hand psoriasis looks like,
how to cleanse and moisturize without making flares worse, and how to protect your hands
with gloves, smart product choices, and trigger management. You’ll also see how photos,
routines, and real-world experiences can support the treatment plan you build
with your dermatologist, so your hands feel more like your own again.






