Table of Contents >> Show >> Hide
- What is electrical muscle stimulation?
- EMS, TENS, FES: what’s the difference?
- How does electrical muscle stimulation work?
- Evidence-based benefits and common uses
- What EMS can’t (realistically) do
- Is electrical muscle stimulation safe?
- What to expect during an EMS session
- At-home EMS devices: smart tool or expensive gadget?
- Practical tips if you’re curious about EMS
- Real-world experiences and lessons from EMS therapy
- The bottom line
If you’ve ever seen someone in physical therapy hooked up to little sticky pads
that make their muscles twitch and thought, “Uh… are they being gently
electrocuted?” you’ve already met electrical muscle stimulation.
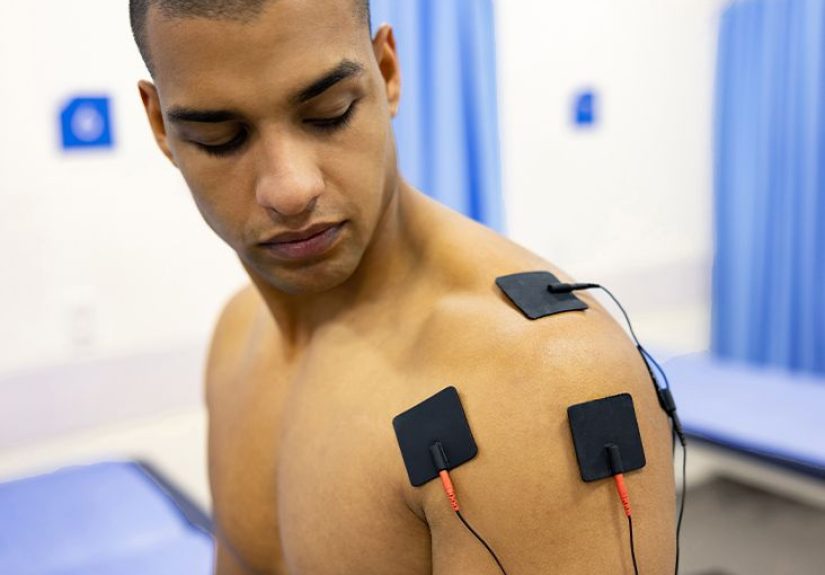
Electrical muscle stimulation (EMS) is a therapy that uses small,
controlled electrical pulses to make muscles contract. It’s used in
rehabilitation after injuries, to help manage pain and stiffness, and
sometimes in fitness settings to supplement workouts. It can be helpful for
many people but it’s not a magic six-pack machine, and it’s definitely not
for everyone.
In this in-depth guide, we’ll break down what EMS is, how it works, what the
evidence actually says, who may benefit, who should avoid it, and what to
know before you buy that “get ripped on your couch” belt you saw in an ad.
What is electrical muscle stimulation?
Electrical muscle stimulation (often shortened to EMS or NMES for
neuromuscular electrical stimulation) uses a device that sends gentle
electrical impulses through electrodes placed on your skin. These impulses
trigger your muscles to contract and relax, a bit like they would during
regular exercise just with less sweat and more wires.
Clinically, EMS is often used:
- In physical therapy and rehab clinics
- After surgeries such as knee or hip replacements
- After injuries where a muscle has been weak or immobilized
- As part of neurological rehab (for example, after a stroke)
The core idea is simple: if a muscle isn’t working well because of
weakness, injury, or nerve issues EMS can help recruit and activate those
muscle fibers in a controlled way.
EMS, TENS, FES: what’s the difference?
Electrical stimulation comes in several flavors, and the acronyms can get
confusing fast. Here’s a quick breakdown of the most common types you’ll
hear about.
EMS / NMES (electrical muscle stimulation)
EMS or NMES is designed to stimulate muscles directly. The device sends
pulses that make muscles contract, which can:
- Help maintain or improve muscle strength
- Reduce or prevent muscle atrophy (muscle wasting)
- Assist with muscle re-education after injury or surgery
- Support circulation and reduce stiffness
Functional electrical stimulation (FES)
Functional electrical stimulation is a subtype of EMS used mostly in
neurological rehab, such as after a spinal cord injury or stroke. The goal
is not just to make muscles contract, but to make them contract in a way
that performs a specific function like lifting the foot during walking or
opening the hand to grasp an object.
FES is often used to:
- Improve walking patterns (gait)
- Help with arm and hand function
- Maintain muscle mass in weakened limbs
TENS (transcutaneous electrical nerve stimulation)
TENS is related but different. Instead of primarily targeting muscles, TENS
machines send currents that focus on nerves to help manage pain. A TENS
unit is often used for:
- Chronic back pain or neck pain
- Arthritis pain
- Post-surgical discomfort
In short: EMS is mainly for muscle activation and strength; TENS is mainly
for pain relief. Some devices combine both modes, which is great as long
as you know which mode you’re actually using.
How does electrical muscle stimulation work?
Your muscles contract when nerves send them electrical signals. EMS simply
mimics that signal from the outside. Sticky electrode pads are placed over
the muscle group (for example, the quadriceps on the front of your thigh),
and the device sends short pulses at controlled intensities and frequencies.
These pulses:
- Activate motor nerves, which tell the muscle fibers to contract
- Recruit muscle fibers that might be “lazy” or underused
- Can be dialed up or down depending on your tolerance and goals
Interestingly, EMS can sometimes recruit fast-twitch muscle fibers (the
powerful, quick-contracting ones) differently than voluntary exercise. That
has led to research into EMS for athletic training and performance though
the real-world benefits vary and depend a lot on how it’s used, the
protocol, and what you compare it to.
Evidence-based benefits and common uses
1. Rehab after injury or surgery
One of the most established uses of EMS is in physical therapy settings. If
you’ve had knee surgery, ligament repairs, or a long period in a cast, the
muscles around the joint can weaken surprisingly fast. EMS can be used
alongside exercises to:
- Strengthen muscles that are hard to activate on their own
- Improve range of motion
- Help retrain normal movement patterns
For example, after knee surgery, it’s common for the quadriceps to “shut
down” and be difficult to contract fully. EMS can help “wake up” that
muscle while a person practices simple leg lifts or knee extensions.
2. Preventing or slowing muscle atrophy
When a limb is immobilized think casts, long hospital stays, or severe
weakness muscles can shrink and lose strength quickly. EMS can help slow
this muscle loss by causing regular contractions even when a person can’t
fully move on their own.
Research has looked at EMS for people with heart failure, chronic illness,
and those in intensive care, where even small improvements in muscle mass
and function can make a big difference in recovery and independence.
3. Supporting people with neurological conditions
In conditions like stroke, spinal cord injury, or multiple sclerosis,
nerves don’t always communicate normally with muscles. Functional electrical
stimulation (FES) can help:
- Improve walking by lifting the foot at the right time in the step
- Assist with reaching, grasping, or opening the hand
- Maintain muscle bulk and joint mobility in weak limbs
While FES doesn’t “cure” the underlying condition, it can improve function,
make daily tasks easier, and support ongoing rehab efforts.
4. Pain management and stiffness
EMS is not purely a pain therapy (that’s more the territory of TENS), but
muscle stimulation can still help with discomfort. By increasing circulation
and reducing muscle spasm, EMS can:
- Ease muscle tightness after injury or overuse
- Reduce the feeling of stiffness around joints
- Support overall comfort when used alongside stretching and exercise
Some devices and protocols combine EMS with TENS-style pain control, giving
both muscle activation and nerve-level pain relief.
5. Athletic training and performance
EMS has made its way into sports performance and boutique “20-minute EMS
workout” studios. The idea is that by contracting more muscle fibers at once
and layering EMS on top of voluntary exercise, you might:
- Boost strength gains
- Improve endurance in specific muscle groups
- Assist recovery between training sessions
The evidence is mixed. Some studies suggest EMS can be a helpful supplement
to traditional training, especially when time is limited or a specific
muscle group is lagging. But it’s not a substitute for real-world movement,
skill practice, and regular exercise. Think of EMS as a side dish, not the
main course.
What EMS can’t (realistically) do
Let’s talk about the elephant in the room: those slick ads promising “rock
hard abs in 2 weeks while you watch TV.” EMS is useful, but it’s not magic.
Here’s what electrical muscle stimulation is unlikely to do on its own:
- Give you a six-pack without overall exercise and nutrition changes
- Melt fat directly off your belly, thighs, or arms
- Replace full-body strength training or cardio workouts
In the U.S., the Food and Drug Administration (FDA) regulates EMS devices as
medical devices. That means manufacturers can’t legally claim that their
devices will reshape your body, build huge muscles, or cure diseases unless
those claims are backed by evidence and cleared through the proper channels.
Bottom line: EMS can help support muscle tone and strength, especially in a
rehab or training context. It’s a helpful tool, not a shortcut to skipping
leg day forever.
Is electrical muscle stimulation safe?
For many people, EMS is considered generally safe when used as directed and
under the guidance of a qualified professional. Most people describe the
sensation as a strong tingling or firm pulsing that can feel strange but
shouldn’t be painful.
That said, this is still an electrical current going through your body, and
there are important safety rules and contraindications.
People who should not use EMS without medical clearance
-
Anyone with a pacemaker or implanted defibrillator (or
other implanted electronic devices). EMS can interfere with these devices
and may be dangerous. -
People with certain cardiac conditions, especially if
electrodes would be placed near the chest. -
Pregnancy, particularly over the abdomen or lower back
(unless a healthcare professional specifically approves a protocol). -
Areas with unstable fractures (the muscle contractions
may disturb the fracture). -
Active infection, open wounds, or severe skin irritation
where the electrodes would be placed. -
Known or suspected malignancy directly under the treatment area,
unless cleared by oncology and rehab teams. -
Severe peripheral vascular disease or blood clots in the
region to be treated.
Situations where extra caution is needed
EMS may still be used in some of these situations, but only with careful
medical supervision:
- People with epilepsy (especially if using EMS near the head or neck)
- Children or older adults with fragile skin or limited sensation
- People with reduced feeling in an area (risk of burns or over-stimulation)
- Areas over metal implants or fixation devices
As with any therapy, a thorough medical history and proper screening are key
before starting electrical stimulation especially for home use.
What to expect during an EMS session
If you’re receiving EMS in a clinic, a typical session might look like this:
-
Assessment. Your physical therapist or clinician reviews
your medical history, goals, and any contraindications. -
Electrode placement. They clean the skin and place
electrodes over targeted muscles (for example, quadriceps, hamstrings, or
shoulder muscles). -
Setting intensity. The current is turned up gradually
until you feel a strong, but tolerable, contraction. You may see the
muscle visibly twitch or hold a contraction. -
Active participation. You’re often asked to contract the
muscle at the same time, or perform simple movements, so the stimulation
supports normal function. -
On-off cycles. The machine typically runs in cycles
(e.g., 10 seconds on, 20 seconds off) to avoid fatigue. -
Duration. A session may last 10–20 minutes for a
particular muscle group, often combined with other exercises and manual
therapy.
After the session, the muscle may feel like it had a workout a bit tired,
maybe mildly sore the next day. That’s usually normal, but any sharp or
lingering pain should be reported to your provider.
At-home EMS devices: smart tool or expensive gadget?
Over-the-counter EMS units are widely available and marketed for fitness,
recovery, and pain relief. If you’re considering one, keep these points in
mind:
-
Check for regulatory clearance. In the U.S., look for
FDA-cleared devices and read what they’re actually cleared for
(e.g., muscle toning vs. pain relief vs. rehab support). -
Read the manual. Yes, really. Follow guidelines on
electrode placement, intensity, session length, and contraindications. -
Start low and go slow. Begin at a low intensity and build
up gradually. More is not always better especially with electricity. -
Use it as a complement, not a replacement. EMS works best
alongside active exercise, stretching, and strength training, not instead
of them. -
Talk to your healthcare provider first if you have any
medical conditions, past surgeries, implanted devices, or are pregnant.
Practical tips if you’re curious about EMS
-
Start with a professional. If possible, try EMS in a
physical therapy or rehab setting first. You’ll learn proper placement,
safe intensity levels, and realistic expectations. -
Pair EMS with movement. Combining EMS with simple
exercises (like straight leg raises, sit-to-stand, or arm lifts) often
works better than passive stimulation alone. -
Monitor your skin. Check for redness, irritation, or
burns after sessions. Rotate electrode placement as recommended. -
Track your progress. Pay attention to changes in strength,
function, or pain levels over several weeks, not just one session. -
Be skeptical of big promises. If a product claims to
“replace your workout” or “melt fat,” that’s a red flag. EMS is a tool to
support your program, not a miracle device.
Real-world experiences and lessons from EMS therapy
While research studies give us the big-picture data, real-world experiences
help illustrate what electrical muscle stimulation actually feels like in
everyday life. Here are some common patterns people report when EMS is used
appropriately and consistently.
Recovering from surgery: the “wake-up call” for sleepy muscles
Imagine someone who just had knee surgery. In the first days and weeks,
simply tightening the quadriceps can feel nearly impossible. The brain is
willing, but the muscle doesn’t quite get the memo. When EMS is added to
early rehab, many patients describe it as a “reminder” to the muscle the
stimulation helps them feel where the muscle is and what a full contraction
is supposed to be like.
Over several sessions, they often notice:
- They can contract the muscle better even without the machine
- It’s easier to perform basic exercises like straight leg raises
- Walking and climbing stairs start to feel more stable
EMS doesn’t replace the hard work of rehab, but it can shorten that awkward
phase where everything feels weak and unresponsive.
Living with neurological conditions: small gains that matter a lot
For people with stroke or spinal cord injury, EMS and FES can be part of a
long-term plan to maintain function. For example, a person with “foot drop”
where the foot drags during walking might use FES to lift the foot at
the right moment in each step. Over time, this can reduce tripping, improve
confidence, and make community walking more realistic.
Others may use EMS to:
- Help open and close the hand for grasping objects
- Maintain muscle mass in a limb that’s weaker or partially paralyzed
- Work on sitting balance and posture by activating core muscles
These improvements may seem small on paper, but being able to walk to the
mailbox, hold a cup, or transfer more easily can be huge for independence
and quality of life.
Adding EMS to fitness: useful boost, not a magic button
In fitness studios and home gyms, some people enjoy adding EMS sessions to
their weekly routine especially if they:
- Feel certain muscles don’t “turn on” well during workouts
- Have imbalances between sides (for example, one quad weaker after an old injury)
- Want extra activation without increasing joint load
A common experience is that EMS helps them feel their muscles more clearly
during strength exercises. For example, using EMS on the glutes during
bridges or squats can make it easier to focus on those muscles instead of
letting the lower back or hamstrings dominate.
However, people who rely only on EMS and ignore overall training, sleep,
nutrition, and recovery usually end up disappointed. The best results show
up when EMS is plugged into a well-rounded plan not used as a stand-alone
hack.
When EMS doesn’t help as much as hoped
It’s also true that EMS is not a game-changer for everyone. Some people:
- Find the sensation too uncomfortable, even at low settings
- Don’t notice much difference in pain levels compared with other strategies
- Realize that practical barriers (time, setup, cost) make it hard to use consistently
In those cases, therapists may shift the focus toward other treatments such
as targeted exercise, manual therapy, medication adjustments, or different
pain-management approaches. EMS is just one option in a large toolkit not
the only route to recovery.
Key takeaways from real-world EMS use
- Consistency over weeks, not days, matters most.
- EMS tends to work best when you’re actively involved, not just lying there.
- Clear goals (walk better, strengthen a muscle, manage stiffness) help guide protocols.
- Honest communication with your provider about comfort and expectations is crucial.
Taken together, both research and real-world experience suggest that
electrical muscle stimulation can be a valuable helper especially in rehab
and targeted training as long as it’s used safely, intentionally, and as
part of a bigger plan for your health.
The bottom line
Electrical muscle stimulation is a well-established therapy that uses
controlled electrical pulses to activate muscles, support strength and
function, and complement rehab and training. It’s not a shortcut to instant
abs, but it can be a powerful ally when used thoughtfully, especially under
professional guidance.
If you’re curious about EMS, talk with your healthcare provider or physical
therapist. They can help you decide whether it fits your goals, your
medical history, and your overall game plan and how to use it safely if
it does.