Table of Contents >> Show >> Hide
- Chickenpox in 2026: Why Are We Still Dealing With This?
- What Chickenpox Actually Looks Like (And Why It Can Fool You)
- The Truly Scary Part: Complications and Higher-Risk Groups
- How Chickenpox Spreads Like Gossip (But With a Longer Memory)
- The Vaccine Story: From “Everybody Gets It” to “Mostly Preventable”
- If Chickenpox Shows Up at Your House: A Practical Game Plan
- The Social Side of the Problem: Parties, Myths, and Misplaced Nostalgia
- What “Winning” Against Chickenpox Looks Like: A Simple Checklist
- Experiences From the Front Lines (About )
- Conclusion
Chickenpox used to be the childhood “rite of passage” nobody asked forlike braces, but itchier.
Then the vaccine arrived, and many of us mentally filed varicella under “solved problems,” right next to dial-up internet and carrying paper maps.
Except… chickenpox didn’t get the memo. It’s far less common than it used to be, but it still shows up in families, schools, and group settingsoften
at the worst possible time (holidays, exams, that week you finally scheduled a haircut).
This is our terrifying chickenpox problem in a nutshell: the disease is usually mild in healthy kids, which makes it easy to underestimate.
But it’s also highly contagious, can be serious in higher-risk people, and creates chaos when it collides with modern lifechild care policies,
missed work, vulnerable relatives, and the occasional social-media “hot take” that treats a vaccine like optional software updates.
Let’s unpack what chickenpox is today, why it still matters, what “breakthrough chickenpox” means, and how to handle it without turning your home
into a scratchy, sleepless reality show.
Chickenpox in 2026: Why Are We Still Dealing With This?
Chickenpox (varicella) is caused by the varicella-zoster virus (VZV). It spreads easily, especially in close-contact settings like homes, classrooms,
and sports teams. The good news is that the U.S. vaccination program has been a public-health success storydramatically reducing cases, severe illness,
hospitalizations, and deaths compared with the pre-vaccine era.
The not-so-fun news: “reduced” doesn’t mean “gone.” Chickenpox can still pop up when:
- Vaccination is delayed or skipped (even in pockets).
- People miss the second dose and have weaker protection than they could.
- Breakthrough cases happen (yes, even after vaccinationusually milder, but still contagious).
- Teens and adults who never got vaccinated or never had chickenpox get exposed later in life, when illness can be more severe.
- High-risk people (pregnant individuals, immunocompromised family members) are in the same community, raising the stakes.
So, the “terrifying” part isn’t just the rashit’s the ripple effect. Chickenpox can force quarantine decisions, trigger notifications to schools and
teams, and create high-stress situations for families with medically vulnerable members.
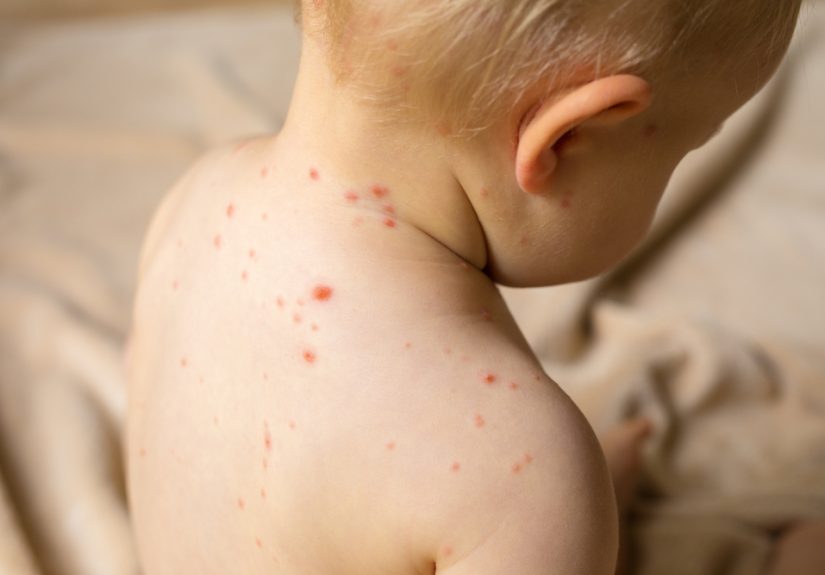
What Chickenpox Actually Looks Like (And Why It Can Fool You)
Classic chickenpox often starts with a general “blah” feelingmild fever, tiredness, reduced appetitefollowed by an itchy rash that comes in waves.
In many kids, it’s uncomfortable but manageable at home with supportive care and a lot of patience.
Breakthrough chickenpox: the sneaky version
Some vaccinated people still get chickenpox. This is called breakthrough varicella. The plot twist is that breakthrough cases
often look different: fewer spots, sometimes more like red bumps than classic fluid-filled blisters, and milder symptoms overall.
That’s great for the patientbut confusing for everyone trying to figure out whether it’s chickenpox, bug bites, or “mystery rash #47.”
Here’s the key: milder doesn’t mean “not contagious.” Breakthrough cases can still spread VZV, especially around people who aren’t immune.
Translation: don’t rely on “it doesn’t look that bad” as your infection-control plan.
The Truly Scary Part: Complications and Higher-Risk Groups
In healthy children, chickenpox is often mild. But complications can happen, and certain groups have a higher risk of severe disease. The stakes go up
for:
- Infants (especially those too young to be vaccinated).
- Adolescents and adults (illness is more likely to be more intense than in younger kids).
- Pregnant people (risk considerations are differentmedical guidance matters fast).
- People with weakened immune systems (including some cancer treatments, transplant patients, advanced HIV, and certain medications).
Potential complications include bacterial skin infections (often from scratching), dehydration, and more serious issues like pneumonia or inflammation
involving the nervous system. Most families never experience those outcomesbut “rare” is not the same as “impossible,” especially when someone in a
household is medically vulnerable.
Aspirin and chickenpox: a hard no
One of the most important safety rules is simple: do not give aspirin to children with chickenpox. If fever relief is needed, families
are commonly advised to use non-aspirin options and follow clinician guidance. Also, some pediatric guidance recommends avoiding ibuprofen when possible
during chickenpox because of an association with serious bacterial skin infections.
How Chickenpox Spreads Like Gossip (But With a Longer Memory)
Chickenpox spreads easily through respiratory droplets/aerosols and direct contact with fluid from lesions. The tricky part is timing: a person can be
contagious before the rash becomes obviousso by the time you think, “Huh, that’s a suspicious spot,” the virus may already have done
a few laps around the household.
In close-contact settings, the virus is extremely efficient. In other words: if someone isn’t immune and spends a lot of time near an infectious person,
the odds of transmission are high.
The Vaccine Story: From “Everybody Gets It” to “Mostly Preventable”
The best way to prevent chickenpox is vaccination. In the U.S., varicella vaccine is routinely given in two doses during childhood.
This two-dose approach is designed to improve protection and reduce breakthrough cases compared with a single dose.
MMR + varicella vs. the combo shot (MMRV): why families hear mixed messaging
Parents may encounter two different formats:
separate vaccines (MMR and varicella) or the combined MMRV vaccine.
Protection against measles, mumps, rubella, and varicella is considered comparable between these approaches. The difference is mainly about
practical considerations and side-effect profiles for certain agesparticularly a small increased risk of febrile seizures after the first MMRV dose
in younger children compared with giving MMR and varicella separately at the same visit.
In late 2025, CDC communications and provider guidance emphasized using separate MMR and varicella vaccines for the first dose in younger children,
while still allowing MMRV in some circumstances (such as if parents specifically prefer it). Because vaccine guidance can evolve, the most reliable move
is to check the current CDC schedule and discuss options with a pediatric clinician.
Vaccination doesn’t just protect one kidit protects the calendar
A vaccinated community has fewer outbreaks, fewer “everyone stay home” situations, and fewer anxious calls to grandparents who are immunocompromised.
It also reduces the odds of chickenpox showing up later in adulthood, when it tends to hit harder.
If Chickenpox Shows Up at Your House: A Practical Game Plan
If you suspect chickenpox, your first job is to reduce spread and get appropriate medical guidanceespecially if anyone in the household is high-risk.
Here’s a common-sense approach many clinicians recommend:
1) Call ahead before going in
Chickenpox spreads easily. If a clinic visit is needed, call first so the office can protect other patients (especially infants and immunocompromised
people in waiting rooms).
2) Stay home until no longer contagious
Exclusion guidance often focuses on staying home until lesions have crusted over. For vaccinated people who don’t develop classic crusting lesions,
guidance may instead focus on the point when no new lesions have appeared for a set period (often discussed as 24 hours). Schools and child care
programs may follow public-health recommendations and local rules.
3) Treat symptoms safely
- Itch control: cool baths, colloidal oatmeal baths, calamine lotion, loose clothing, and short nails can help reduce scratching.
- Fever relief: follow clinician guidance; avoid aspirin in children with chickenpox.
- Hydration: keep fluids easy and frequent (popsicles count as diplomacy).
4) Ask about antivirals if someone is higher-risk
Antiviral medication (such as acyclovir) may be considered for people at higher risk of complications. Timing matters; clinicians often emphasize that
antivirals work best when started early after rash onset. This is not a DIY decisioncall a clinician quickly if risk factors are present.
5) Post-exposure steps can matter
If someone without evidence of immunity is exposed, clinicians may recommend vaccination soon after exposure to prevent or reduce illness.
For certain high-risk exposed individuals, a special immune globulin product may be considered. The right option depends on age, immune status, and
medical historyso this is another “call the clinician” moment, not a social-media poll moment.
The Social Side of the Problem: Parties, Myths, and Misplaced Nostalgia
Every few years, “chickenpox parties” reappear in the public conversationusually framed as a wholesome throwback to the era when we also thought
Jell-O salad was cuisine. Intentionally exposing kids is risky because you can’t predict who will develop complications, and you may inadvertently
expose infants, pregnant people, or immunocompromised community members.
Modern prevention is less dramatic and far more effective: vaccinate on schedule, catch up if you missed doses, and treat chickenpox like the contagious
illness it isnot a quirky childhood milestone.
What “Winning” Against Chickenpox Looks Like: A Simple Checklist
- Know your household’s immunity status: two-dose vaccination or prior disease history (as assessed by a clinician) matters.
- Plan for school/child care rules: ask how they handle varicella notices and return policies.
- Protect high-risk relatives: don’t “wait and see” if a vulnerable person might have been exposedcall a clinician quickly.
- Use safe fever/itch strategies: no aspirin for kids with chickenpox.
- Normalize prevention: vaccines are boring in the best waybecause they prevent the chaos.
Experiences From the Front Lines (About )
If you’ve never lived through chickenpox in a household, it’s hard to explain the vibe. It’s like hosting a tiny, itchy gremlin who looks exactly like
your kid, sounds exactly like your kid, and somehow has the power to make time slow down. Parents don’t remember chickenpox in minutes or hours; they
remember it in “waves.” The first wave is denial: “Maybe it’s just a rash.” The second wave is acceptance: “Okay, that’s… definitely chickenpox.”
The third wave is logistics: school emails, childcare calls, calendar cancellations, and the sudden realization that you do not own enough clean pajamas
to get through a week of interrupted sleep.
One common experience families talk about is the nighttime itch spiral. During the day, distraction does a lot of heavy liftingcartoons, books, snacks,
the sacred power of screen time. But at night, when everything is quiet, the itch seems louder. Parents become part nurse, part negotiator, part
professional “please don’t scratch” coach. You find yourself trimming nails like you’re preparing a tiny athlete for competition. You learn that
“loose, breathable clothing” is not a cute lifestyle suggestion; it’s survival gear. And you discover that a cool bath at 2 a.m. can feel like both
a miracle and a personal failure of modern medicine. (It’s neither. It’s just chickenpox being chickenpox.)
Another experience: the social ripple effect. The moment you notify a school or team, your phone becomes a notification center for other people’s
anxiety. A parent asks, “My baby is too young for the vaccineshould I panic?” Someone else says, “We’re visiting Grandma this weekendwhat do we do?”
And that’s when chickenpox stops being a private inconvenience and becomes a community problem. Families with immunocompromised relatives often describe
a special kind of stressnot because they’re dramatic, but because they understand that “mild for most kids” is not a guarantee for everyone.
Breakthrough chickenpox brings its own weirdness. The rash might be lighter, and the child might feel mostly okay, which tempts people to treat it like
“no big deal.” But parents quickly learn that “no big deal” ends the moment someone else’s unvaccinated toddler is in the same play space. Many families
end up feeling like they’re doing detective work: counting spots, tracking new bumps, comparing photos day-to-day (while trying not to become the kind
of person who sends rash updates to group chats).
And then there’s the relief on the other sidewhen the household finally turns the corner. The itch fades. The energy comes back. The child stops
looking like a tiny constellation of red dots. Parents restock the laundry basket, delete the “chickenpox plan” notes from their phones, and swearvery
calmly, very sincerelythat they will never again underestimate a “common childhood illness.” Because the terrifying chickenpox problem isn’t just the
virus. It’s the way a small infection can hijack a whole family’s week, stress a whole community, and remind us that prevention is usually cheaper than
chaos.
Conclusion
Chickenpox is far less common in the U.S. than it used to be, but it hasn’t vanishedand it still has the power to disrupt families and endanger
higher-risk people. The smart response is equal parts prevention and preparedness: follow recommended vaccination guidance, recognize that breakthrough
cases can still spread, and handle suspected cases with practical isolation and safe symptom care. If there’s one takeaway, it’s this: chickenpox isn’t
a nostalgic childhood milestone. It’s a preventable public-health problem that we can keep shrinkingone routine vaccine visit at a time.