Table of Contents >> Show >> Hide
- What Is TMS, Exactly?
- How Could TMS Help Migraine?
- Potential Benefits of TMS for Migraine
- Effectiveness: What the Evidence Suggests (and What It Doesn’t)
- Who Might Be a Good Candidate?
- What Does Treatment Feel Like?
- Precautions, Risks, and Side Effects
- Practical Stuff: Cost, Insurance, and Access
- How to Give TMS a Fair Trial (Without Gaslighting Yourself)
- Real-World Experiences (500+ Words): What People Often Notice, Feel, and Learn
- Experience #1: The first week is mostly about logistics
- Experience #2: Sensations varymost are mild, a few are annoying
- Experience #3: “It didn’t stop the migraine, but it changed the migraine”
- Experience #4: Preventive use feels boring… until you look back at the calendar
- Experience #5: The best results usually come from a complete plan, not a single gadget
- Conclusion
Migraine is the kind of overachiever that doesn’t just bring head painit can bring nausea, light sensitivity,
brain fog, and the delightful feeling that your skull is hosting a drum circle. So when people hear “TMS”
(transcranial magnetic stimulation), their first question is usually: “Is this the part where I become a superhero?”
Sadly, no cape is included. But for certain migraine patients, TMS can be a legitimate, non-drug toolespecially
if you want options beyond “try another pill and hope your stomach forgives you.”
This article synthesizes medical and regulatory information from U.S. sources (including the FDA, major health systems,
professional headache organizations, and peer-reviewed research indexed by NIH/PubMed).
What Is TMS, Exactly?
Transcranial magnetic stimulation (TMS) uses magnetic pulses to influence nerve activity in the brain.
It’s noninvasive (no surgery), and for many people it’s a “sit there and let the machine do the work” kind of therapy.
Important: “TMS for depression” and “TMS for migraine” aren’t always the same thing
When most people hear “TMS,” they picture in-clinic treatments for depression that target the front of the head
over multiple sessions. Migraine-focused TMS often refers to single-pulse TMS (sTMS), which is typically
applied at the back of the head (near the occipital region). In other words: same broad family, different game plan.
sTMS vs. rTMS: Two cousins, different personalities
-
sTMS (single-pulse TMS): A brief magnetic pulse, often used with a portable device and sometimes used
at home (with a prescription). It’s commonly discussed in migraine neuromodulation. -
rTMS (repetitive TMS): A sequence of pulses delivered in a session, often in clinics. It’s well-known
in psychiatry and is being studied for migraine prevention protocols.
How Could TMS Help Migraine?
Migraine isn’t “just a headache.” It involves changes in brain excitability and pain pathways. One migraine concept
you’ll hear in neuromodulation discussions is cortical spreading depressiona wave of altered brain activity
that’s strongly linked to migraine aura and may also play a role in attack biology.
The basic idea behind TMS for migraine is that a magnetic pulse can nudge brain activity away from the “migraine launch sequence.”
Think of it as tapping the brakes on an overexcited nervous systemideally early, before the attack fully commits.
Potential Benefits of TMS for Migraine
1) A non-drug option (with a different side-effect profile)
Some people want fewer medicationsbecause of side effects, interactions, pregnancy planning, rebound headaches,
or because they’ve already tried half the pharmacy aisle. Neuromodulation can be appealing because it’s not a pill
and doesn’t rely on digestion, liver metabolism, or perfect timing with food.
2) Can be used “as needed” (depending on device and plan)
With migraine neuromodulation, some approaches are used at the first sign of an attack, while others are used daily
as prevention. Your clinician’s guidance matters here because protocols vary by device type and migraine pattern.
3) May reduce reliance on rescue meds for some patients
Even when TMS isn’t a magical off-switch, some patients use it as part of a layered planpotentially lowering how often
they need triptans, NSAIDs, or other rescue treatments. That can be a big deal if you’re trying to avoid medication overuse headache.
4) A “toolbox” approach that plays well with others
Migraine treatment often works best as a system: lifestyle triggers, sleep, hydration, preventive strategies,
acute treatments, and sometimes devices. TMS can be one of those toolsespecially for people who want flexibility.
Effectiveness: What the Evidence Suggests (and What It Doesn’t)
Let’s be honest in the most helpful way: TMS for migraine is promising, but it’s not a guaranteed win for everyone.
Response depends on migraine type (with aura vs. without), attack frequency, how early you treat, and individual biology.
Acute treatment (stopping or reducing an attack)
The strongest migraine-specific “TMS device” story in the U.S. has historically been around sTMS for acute migraine,
originally cleared for migraine with aura. In real life, that tends to mean:
- Best results are often reported when used early in an attack (or at aura onset, if you get aura).
- Some people get meaningful pain reduction; others get partial relief; some get none.
- It may be especially relevant for patients who can’t take certain medications or want fewer meds.
Prevention (reducing monthly migraine days)
Preventive use is typically about consistencydaily sessions according to a prescribed plan. Research on rTMS and
sTMS prevention is still evolving, and results vary by protocol (target area, frequency, number of sessions).
A practical way to think about prevention outcomes: you’re usually not looking for “zero migraine forever.”
You’re looking for fewer migraine days, less intense attacks, shorter duration, or
improved function (fewer lost workdays, fewer “cancelled plans” moments).
So… is it “clinically effective”?
For some people: yes, it can be a meaningful part of care. For others: it’s a swing-and-a-miss.
If your migraine pattern is complex (chronic migraine, multiple triggers, medication overuse, comorbid anxiety/sleep issues),
your clinician may frame TMS as an adjunct rather than a solo hero.
Who Might Be a Good Candidate?
TMS may be worth discussing with a headache specialist if you:
- Have migraine (especially if you experience aura), and want non-drug acute options
- Can’t tolerate or shouldn’t use certain medications
- Want to reduce reliance on rescue meds
- Have tried standard preventives and still have frequent migraine days
- Prefer a device-based, “do-it-early” strategy
It may be less compelling if you’re looking for an instant cure, dislike routines (daily preventive sessions require consistency),
or have contraindications that make magnetic stimulation unsafe.
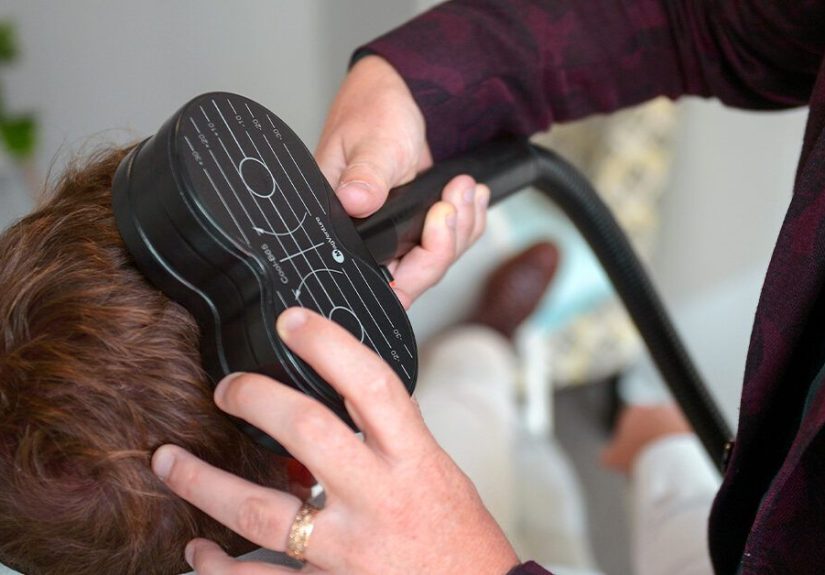
What Does Treatment Feel Like?
For in-clinic rTMS-style sessions
In a clinic setting, you typically sit in a chair while a clinician positions a coil. You may feel tapping sensations,
mild scalp discomfort, or facial muscle twitching. Some people get a temporary headache afterward; many find side effects
fade as they get used to sessions.
For at-home, migraine-directed sTMS-style use (when prescribed)
At-home use is often designed to be quick and repeatable. The big “success factor” here is timing:
using it early, following the prescribed number of pulses, and tracking results so your clinician can tweak the plan.
Precautions, Risks, and Side Effects
TMS is generally well-tolerated, but “generally” is not the same as “for everyone.” The most common issues are usually
mild and short-lived:
- Scalp discomfort or tenderness
- Headache
- Tingling or facial muscle twitching
- Lightheadedness
The serious (rare) risk: seizure
The most serious potential adverse event with TMS is a seizure. It’s considered rare, and clinics screen for risk factors.
Practical risk reducers include good sleep, avoiding heavy alcohol use, and disclosing any seizure history or brain injury.
Who should be extra cautious (or avoid it entirely)?
This is where you absolutely must follow clinician/device guidance. In general, TMS may be contraindicated if you have:
- Metal in or near the head/neck/upper body that could be affected by magnets
- Implanted electronic devices (some pacemakers, neurostimulators, cochlear implants, etc.)
- A history of seizures or significant seizure risk (this depends on individual factors)
Also: tell your provider about pregnancy, plans to become pregnant, or breastfeeding. Evidence and recommendations can vary,
and the “right” approach depends on the specific device, your migraine severity, and your overall health plan.
Practical Stuff: Cost, Insurance, and Access
Reality check: access can be the hardest part. In-clinic TMS infrastructure is more common for depression than migraine-specific protocols.
Device-based migraine neuromodulation may require prior authorization, rentals/subscriptions, or specific prescribing pathways.
If you’re considering TMS for migraine, ask the office:
- Is this for acute treatment, prevention, or both?
- What outcomes are realistic for my migraine pattern?
- How do we measure successmonthly migraine days, intensity, rescue meds, disability scores?
- What are my contraindications or risk factors?
- What will insurance likely cover, and what will I pay out of pocket?
How to Give TMS a Fair Trial (Without Gaslighting Yourself)
Migraine treatments fail for predictable reasonsbad timing, inconsistent use, unclear goals, or not tracking outcomes.
If you try TMS, do yourself a favor:
- Track migraine days (and rescue meds) for at least 4 weeks before starting.
- Use it the prescribed wayespecially early in attacks if it’s an acute strategy.
- Keep notes: pain level, aura onset, time-to-treatment, and what happened next.
- Reassess at a set checkpoint (often 6–12 weeks for preventive strategies).
Real-World Experiences (500+ Words): What People Often Notice, Feel, and Learn
Let’s talk about the part most articles skip: the “living with it” experience.
Not the glossy brochure versionmore like the day-to-day reality of trying a device while your brain occasionally
believes fluorescent lights are a personal attack.
Experience #1: The first week is mostly about logistics
Many people report that early on, the biggest hurdle isn’t the sensationit’s the routine. Where do you keep the device?
How do you remember to use it at the earliest sign of migraine? What do you do if your aura starts while you’re in a meeting,
in the carpool line, or staring at your inbox like it’s written in ancient runes?
A common “aha” moment is realizing that success often depends on treating early. People who wait until pain is at an 8/10
sometimes describe weaker results than when they treat at 2/10or right when aura begins. The early window can feel inconvenient,
but it’s frequently the difference between “this might be working” and “well, that was anticlimactic.”
Experience #2: Sensations varymost are mild, a few are annoying
Some people describe the sensation as a quick thump or tap. Others notice scalp tenderness or a temporary headache afterward.
A smaller group finds the feeling unpleasant enough that they need adjustments, reassurance, or a different strategy.
The pattern many clinics see with TMS in general is that side effects often get easier over timeyour body learns the routine,
and anxiety about the unknown drops.
Experience #3: “It didn’t stop the migraine, but it changed the migraine”
This is a surprisingly common report in device-based migraine care. Some patients don’t get a full stop, but they notice:
- The attack is shorter
- The peak pain is lower
- Nausea is less intense
- They can delay or reduce rescue medication
- They recover faster the next day
If you measure success only as “pain gone in 20 minutes,” you might miss meaningful gains. Many headache specialists encourage
tracking disability: Did you stay at work? Did you avoid bedrest? Did you function at 70% instead of 10%?
Experience #4: Preventive use feels boring… until you look back at the calendar
Preventive strategies rarely feel dramatic day-to-day. People often describe the first few weeks as “nothing is happening,”
and then they realize they’ve had fewer migraines or fewer “two-day hangover” episodes. That’s why tracking monthly migraine
days is essentialmemory is unreliable, especially when migraine brain is involved.
Experience #5: The best results usually come from a complete plan, not a single gadget
Patients who do best often pair TMS with basics that aren’t glamorous but matter: consistent sleep, hydration, trigger awareness,
treating early, and having a clear medication plan for when a migraine breaks through. It’s not “device vs. meds vs. lifestyle.”
It’s “stack the advantages,” like you’re building a migraine-defense Jenga towerexcept you want it to stay up.
Bottom line: real-world experiences are mixed, but they’re not random. The people who are happiest with TMS tend to have
realistic goals, consistent use, good tracking, and a clinician who treats it as part of a strategynot a miracle.
Conclusion
TMS for migraine sits in the “legit, science-based, not-for-everyone” category. For the right patient, it can be a valuable
non-drug optionespecially as part of a broader plan that includes early treatment, tracking, and smart prevention.
If you’re curious, talk with a headache specialist and bring data (migraine days, triggers, meds used). Migraine responds best
when you treat it like a systemnot like a random lightning strike.