Table of Contents >> Show >> Hide
The Double Marker Test (DMT), also known as the first trimester screening, is a blood test performed early in pregnancy to assess the likelihood of certain fetal conditions, such as Down syndrome and other chromosomal abnormalities. This test, though not diagnostic, provides valuable information to expectant mothers and their healthcare providers. In this article, we will explore what the Double Marker Test is, how it is done, what the results mean, and why it is an important tool in prenatal care.
What Is the Double Marker Test?
The Double Marker Test is a non-invasive prenatal screening test conducted during the first trimester, typically between 9 and 13 weeks of pregnancy. The test measures the levels of two specific proteins in the mother’s blood: pregnancy-associated plasma protein-A (PAPP-A) and human chorionic gonadotropin (hCG). These proteins are produced by the placenta, and their concentrations can provide insights into the likelihood of certain birth defects and chromosomal conditions, such as Down syndrome (Trisomy 21) and Trisomy 18.
How Is the Double Marker Test Done?
The procedure for the Double Marker Test is relatively simple and quick. It involves the following steps:
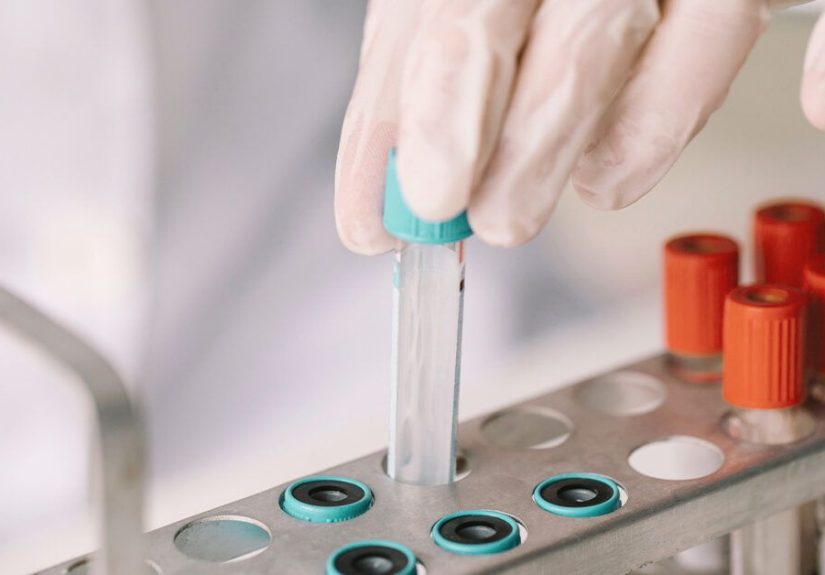
- Blood Collection: A healthcare professional will draw a small sample of blood from the mother’s vein, usually in the arm. This sample will be sent to a laboratory for analysis.
- Analysis: The laboratory will measure the levels of PAPP-A and hCG in the blood. These levels are then compared to a reference range for the mother’s age, gestational age, and other relevant factors.
- Results Interpretation: The test results are used to calculate the risk of chromosomal abnormalities, such as Down syndrome. The results are typically available within a week or two of the blood draw.
What Do the Results Mean?
The results of the Double Marker Test are not definitive and do not diagnose a condition. Instead, the results are presented as a risk ratio. For example, a result might indicate that a particular fetus has a 1 in 100 chance or a 1 in 1,000 chance of having a certain condition, such as Down syndrome. The risk is calculated using a combination of factors, including the blood test results, the mother’s age, and the gestational age of the fetus.
Here’s how the results are generally interpreted:
- Low Risk: If the calculated risk is low, the probability of the baby having a chromosomal abnormality is low. This is typically indicated by a higher PAPP-A level and a lower hCG level.
- High Risk: A high-risk result suggests that the fetus may have an increased likelihood of a chromosomal condition. This is typically indicated by a lower PAPP-A level and a higher hCG level.
- Intermediate Risk: An intermediate risk result falls somewhere between low and high risk. It may indicate that further testing, such as a diagnostic test like amniocentesis or chorionic villus sampling (CVS), is recommended for a more definitive answer.
What Happens After the Test?
If the Double Marker Test shows a high-risk result, it does not mean that the baby has a chromosomal condition. It simply means that there is a higher likelihood compared to the general population. For high-risk results, additional diagnostic tests may be recommended to confirm the presence or absence of any abnormalities. These tests can provide more accurate results, but they are also more invasive and carry a small risk of complications.
If the result is low-risk, the pregnancy is considered to have a low likelihood of chromosomal abnormalities, but the test is not 100% conclusive. The Double Marker Test is just one tool in the broader assessment of fetal health.
Why Is the Double Marker Test Important?
The Double Marker Test provides several benefits for both expectant mothers and healthcare providers. Some key reasons for its importance include:
- Early Detection: Conducting the test early in the pregnancy allows for early detection of potential issues. This can give parents more time to prepare for the possibility of a child with special needs or to make informed decisions regarding the pregnancy.
- Non-Invasive: The test is a simple blood draw, which is less invasive compared to other diagnostic tests, such as amniocentesis or CVS.
- Risk Assessment: It provides a risk assessment rather than a definitive diagnosis, giving parents and doctors the information needed to determine the next steps in prenatal care.
Limitations of the Double Marker Test
While the Double Marker Test is an important tool in prenatal care, it has its limitations:
- Not a Diagnostic Test: As mentioned earlier, the test is a screening tool, not a diagnostic test. A high-risk result does not confirm the presence of a chromosomal abnormality, and a low-risk result does not guarantee a healthy pregnancy.
- False Positives and False Negatives: The test can produce false positives (indicating a problem when there is none) and false negatives (failing to detect an issue that is present). Further testing is necessary to confirm the results.
- Limited Scope: The test is limited to screening for specific chromosomal abnormalities and does not provide information on other potential health issues or birth defects.
Additional Tests to Consider
If the Double Marker Test indicates a high risk of chromosomal abnormalities, additional tests may be recommended, including:
- Non-Invasive Prenatal Testing (NIPT): This test analyzes fetal DNA from the mother’s blood and is highly accurate for detecting conditions like Down syndrome.
- Amniocentesis: A diagnostic test where a small sample of amniotic fluid is taken to analyze the chromosomes of the fetus. This test is more invasive but provides a definitive diagnosis.
- Chorionic Villus Sampling (CVS): A diagnostic test in which a small sample of tissue from the placenta is taken to examine the fetus’s chromosomes. Like amniocentesis, CVS carries a small risk of complications.
Conclusion
The Double Marker Test is an essential prenatal screening tool that provides valuable information about the likelihood of certain chromosomal abnormalities. While the test is not diagnostic, it offers an early opportunity for risk assessment, allowing expectant parents to make informed decisions about their pregnancy. It’s important to remember that the test results are just one piece of the puzzle and that further testing may be necessary to obtain a definitive diagnosis. Expectant mothers should consult with their healthcare provider to understand their results and determine the best course of action for their individual situation.
Experiences with the Double Marker Test
The Double Marker Test is often a point of anxiety for many expectant mothers, particularly when they first learn of its purpose and the implications of the results. However, it’s important to understand that the test is just the beginning of the conversation and not the end of the journey. Many women have shared their experiences of undergoing the test and finding that the results, whether high or low risk, did not necessarily lead to immediate conclusions about the health of their babies.
For example, one woman recounts how her doctor explained the results as a risk assessment rather than a diagnosis. Despite receiving a higher risk result for Down syndrome, further diagnostic testing, including a non-invasive prenatal test (NIPT), provided clearer answers. This second test, which confirmed that her baby was healthy, gave her the peace of mind she needed during a stressful time.
On the other hand, some mothers have had to face the reality of further testing due to a high-risk result. One woman shared that although her Double Marker Test came back with a high-risk ratio for Trisomy 18, she chose to undergo amniocentesis, which confirmed the diagnosis. While the news was difficult, it allowed her to prepare for the birth of a baby with special needs, giving her and her family time to gather the necessary resources and support.
These stories highlight the importance of following up with additional testing and maintaining open communication with healthcare providers. While the Double Marker Test may cause concern, it’s a tool that can help guide the way toward the next steps in ensuring a healthy pregnancy and preparing for any potential challenges.







